Fetal dystocia describes a difficult labor due to the unusual size or position of your fetus. While certain risk factors for dystocia exist, it’s a condition that can show up unexpectedly. Next, Flo offers a complete breakdown of the dystocia meaning and how the issue is typically handled.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Fetal Dystocia: Causes, Contributing Factors, and Treatment Options

Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
What is fetal dystocia?
What is fetal dystocia? The straightforward answer is that it’s a challenging delivery resulting from a larger-than-average baby or awkward positioning.
One of many variations of this condition, shoulder dystocia occurs when your newborn’s head emerges, but one of their shoulders is stuck behind your pubic bone. It happens with approximately 0.7% of vaginal births. Although shoulder dystocia means you’ll require additional medical assistance in the delivery room, your baby can still be born safely and promptly.
Unfortunately, however, fetal dystocia could prove fatal if your child is unable to get through and receives insufficient oxygen for an extended period.
Causes of shoulder dystocia
Many cases of shoulder dystocia go unexplained, but experts believe it’s potentially linked to induced or assisted labors. Particularly lengthy deliveries, or chronic maternal diseases, such as diabetes or obesity, are also occasionally to blame.
Contributing factors for shoulder dystocia
Despite being rather unpredictable, there’s a greater likelihood of shoulder dystocia when the following factors come into play:
- A body mass index (BMI) in the mother of at least 30
- Maternal diabetes
- An unusually long labor
- Induced labor
- Prior pregnancies in which shoulder dystocia was an issue
- Assisted vaginal birth (e.g., those requiring the use of forceps or a vacuum suction apparatus)
- Your fetus is considered heavy for their gestational age
Interestingly enough, some women seem to have no problem giving birth to children weighing over 10 pounds (4.5 kilograms). In fact, roughly half of all cases of shoulder dystocia happen with newborns weighing less than nine pounds (four kilograms).
Note that ultrasound exams cannot confirm fetal size, so they aren’t recommended for detecting shoulder dystocia when none of the above factors are present.
Take a quiz
Find out what you can do with our Health Assistant
Managing fetal dystocia
If your doctor, obstetrician, or midwife suspects you might be susceptible to fetal dystocia, they may suggest a C-section. This is especially suited for pregnant women with diabetes, small pelvises, or a history of dystocia.
The truth is, there’s a possibility of shoulder dystocia in every instance of childbirth. Shoulder dystocia is treated as an emergency situation during which the speed of response is crucial. Your child’s shoulder is preventing the progression of their full birth and must be released as quickly as possible to restore their oxygen supply.
If you experience shoulder dystocia, expect your health care professional to take the following steps:
- Ask you to stop pushing
- Reposition you into the McRoberts maneuver which requires you to lay on your back with your legs pushed outwards and up toward your chest
- Perform an episiotomy, which is making an incision to enlarge your vaginal opening
- Press on your abdomen above the pubic bone to try and release their shoulder
- Ask you to step out of the tub if you have a water birth
Generally speaking, such efforts will allow your child to be born safely. But if these measures fail, your doctor may need to:
- Reach into your vagina in an attempt to free their shoulder
- Have you slowly roll over onto all fours to try and release it
Possible complications of fetal dystocia
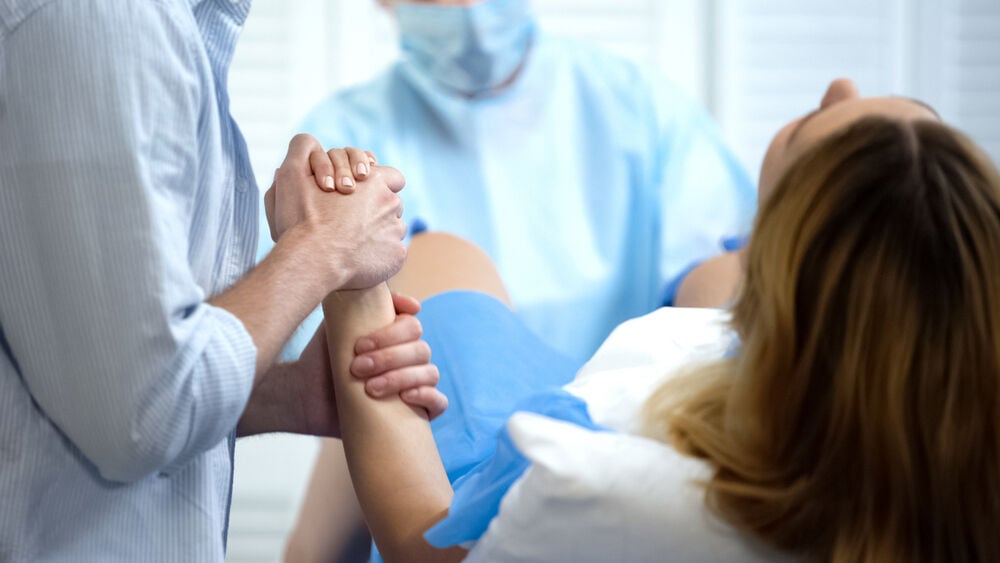
Complications arising from fetal dystocia can directly affect the health of both mother and baby.
Complications for the mother
Not surprisingly, shoulder dystocia often leads to vaginal tears, sometimes extending to your back passage. Depending on severity (first, second, third, or fourth degree), vaginal tearing might warrant stitches. Third and fourth-degree tearing is known to create urinary problems, bowel movement difficulties, pelvic floor dysfunction and prolapse, and painful intercourse.
Shoulder dystocia often leads to vaginal tears, sometimes extending to your back passage.
Postpartum hemorrhaging, which is another term for extremely heavy bleeding after birth, is also common with shoulder dystocia. A blood transfusion or additional treatment may be needed under these circumstances.
Other maternal complications of fetal dystocia include:
- Bladder or uterine rupture
- Cervical tearing
- Symphyseal separation (the separation of normally joined pubic bones)
- Transient lateral femoral neuropathy (damage to a nerve in your thigh)
- Sacroiliac joint dislocation
Complications for the baby
- Approximately 10 percent of newborns experiencing shoulder dystocia will sustain a brachial plexus injury (BPI). The nerves of their neck are stretched, causing loss of movement in one arm. Erb’s palsy is the most common variation of BPI, and it’s usually temporary. Your child’s arm function is restored in no more than a few days, and permanent damage is rare.
- Occasionally, shoulder dystocia is responsible for fractures to your baby’s arm or shoulder. Luckily, these injuries tend to heal on their own, too.
- If the response to shoulder dystocia isn’t swift enough, and their oxygen supply is restricted for too long, it could trigger brain damage.
Future deliveries after dystocia
If you’ve experienced shoulder dystocia in the past, there’s a greater likelihood of it happening again. Discuss with your doctor the various options available to you (e.g., C-section versus vaginal delivery, etc.).
In the event that you were able to quickly release your fetus’ shoulders following dystocia with no other complications, vaginal birth is still an option. Of course, if you or your newborn were injured and/or traumatized, it might be wise to go with C-sections moving forward.
Takeaway
Fetal dystocia is brought on by abnormal fetal size or position and can pose major challenges in the delivery room. As the most frequently occurring type of dystocia, shoulder dystocia is usually handled by health care professionals quickly and decisively, with minimal effect on your newborn’s health.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
History of updates
Current version (03 June 2020)
Published (03 June 2020)
In this article
Get your personal guide to pregnancy with the Flo app
-
Follow your baby's growth week by week
-
Get expert info on symptoms, safe foods, and more
-
Chat with other parents-to-be




