Many things can cause skin changes on the breasts, and it’s normally no big deal. Rarely, it could signal a more serious condition called inflammatory breast cancer (IBC). Keep reading to learn about common causes of breast skin changes; diagnosis and treatment for IBC; what to watch out for; and how to protect your health.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Inflammatory Breast Cancer: How to Spot It and What to Do About It

Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
What can skin changes on the breast mean?
It can be scary to spot a change in your breasts, but if you notice that the skin of your breast is red, swollen, or warm, there’s usually no reason to worry. Breast skin can be quite sensitive, so there are lots of common conditions and causes for breast skin changes, and the vast majority are not too much of a concern.
Some of the most common causes include:
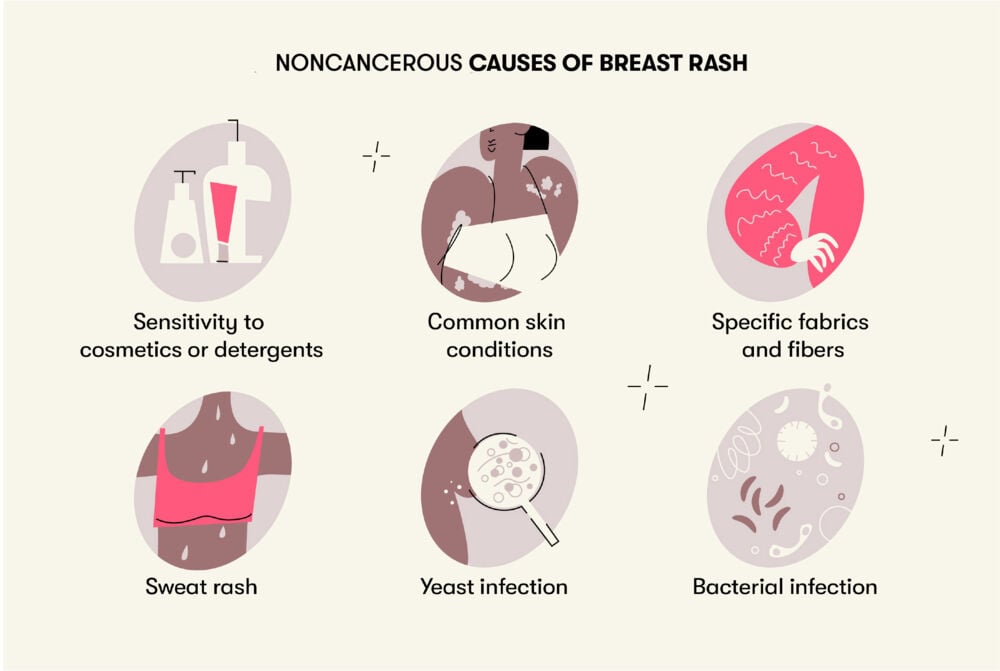
- Sensitivity to cosmetics or detergents — A rash that pops up when you try a new type of body lotion, soap, or laundry detergent could be a mild allergic reaction, which should clear up quickly when you stop using the product that’s causing it.
- Common skin conditions — Eczema and psoriasis can cause a rash, and lots of things can trigger a flare-up, including certain foods, medications, fabrics, chemicals, or simply stress.
- Specific fabrics and fibers — Many people have skin sensitivity to wool and synthetic fibers. For them, wearing clothes made of absorbent fibers, like cotton, can improve the problem. Sleeping in a bra has also been shown to have negative health impacts, including skin irritation and other issues, so your breasts will thank you for letting them breathe at night!
- Sweat rash — Sweat and rubbing can cause a sweat rash. Sweat rash tends to be worse where skin is chafing, making people with larger breasts more prone to developing sweat rash in the creases under their breasts. It usually clears up quite quickly, and showering soon after working out can help.
- Yeast infection — A microscopic fungus called Candida albicans lives on the skin. It’s totally normal, but when there’s too much of it, it can cause a yeast infection. It flourishes in warm, moist areas like the armpits, groin, and creases under the breasts, and it can cause an itchy rash. Taking antibiotics or having diabetes makes you more prone to yeast infections. If the skin under the breast is red, glossy, bumpy, and itchy, a yeast infection could be the culprit. For relief, keep these areas clean and dry. Over-the-counter creams designed specifically for yeast infections usually clear them up quickly.
- Bacterial infection — Sore, cracked skin can harbor bacteria that can lead to infection of the breast skin or milk ducts (mastitis). Make sure to wash your bras frequently and to keep the skin clean and dry. Sometimes, an infection needs to be treated by a health care provider.
Although most of the causes of a rash on the breast aren’t much to worry about, it’s important to be aware of the signs and symptoms of more serious conditions.
What is inflammatory breast cancer?
Inflammatory breast cancer is an aggressive form of breast cancer that usually appears as skin inflammation and general changes in the breast, rather than as a defined lump. IBC is rather rare and only accounts for around one to five percent of diagnosed breast cancers. Educational campaigns about spotting breast cancer early usually focus on the more common forms of breast cancer, which cause lumps and changes in breast tissue that can be felt. But learning about other changes that could signal cancer can help you stay healthy.
Who is at risk?
IBC is more common in females than males, but it’s possible for males to develop it, too. Research tells us that women from African-Caribbean backgrounds have the highest risk of developing IBC, and having a close family member who has had breast cancer is also associated with increased risk. Obesity is another risk factor for IBC.
What are the symptoms?
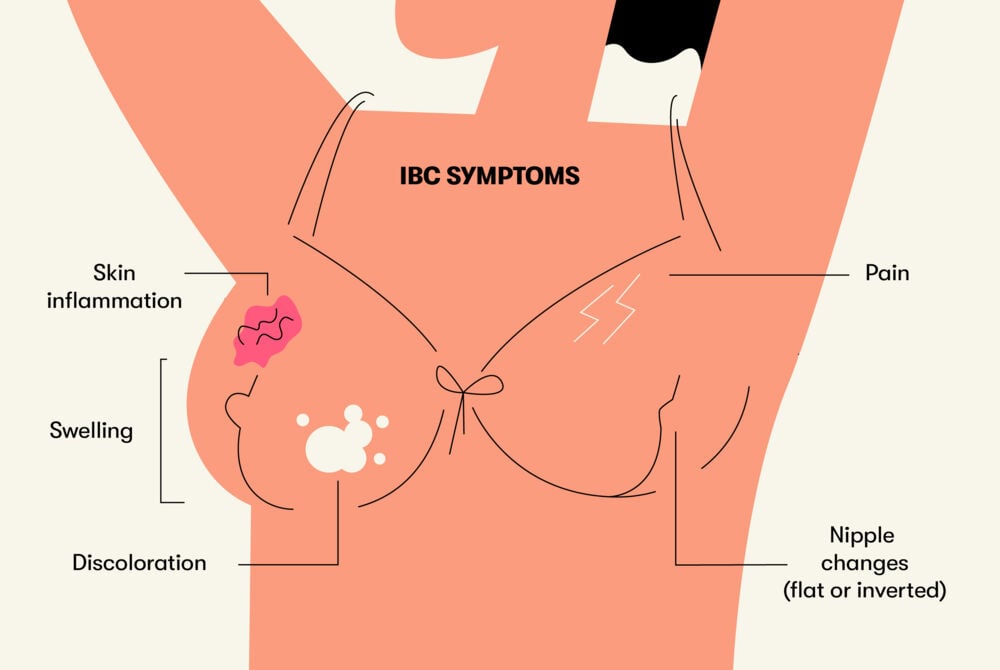
Inflammatory breast cancer can present in a number of ways. The symptoms are persistent and tend to develop relatively quickly (over the course of three to six months). Here’s what to watch for:
- Skin inflammation — The skin of the breast can become warm and puffy and look like the peel of an orange (this is called “peau d’orange”).
- Nipple changes — The nipple can become flat or inverted.
- Swelling — One breast can significantly increase in size.
- Discoloration — The skin of the breast can become very red or almost purple.
- Pain — The breast can become tender.
How to distinguish IBC from other more common conditions
It can be hard to distinguish breast changes caused by inflammatory breast cancer from other common conditions, such as an ordinary rash, allergic reaction, or infection. That’s why it’s important to see a health care provider as soon as you notice any of these changes to figure out the cause and get treatment, if necessary.
Can inflammatory breast cancer be prevented?
Unfortunately, there is no way to prevent IBC (or breast cancer in general). That’s why, in an interview with Flo, breast surgical oncologist Dr. Carlie Thompson says that routine screening for breast cancer is important: It catches breast cancer in its earliest form. Carlie says that the majority of cases of breast cancer are diagnosed via breast cancer screenings, like mammograms. During a mammogram, an x-ray is taken of your breasts to look for abnormal findings that may signify cancer. Mammography can identify cancer years before it could be felt.
The American Cancer Society recommends that women aged 45–54 get annual mammograms.
How is Inflammatory Breast Cancer Diagnosed?
If IBC is suspected because of skin inflammation, nipple changes, or other IBC symptoms, breast imaging — like mammogram, ultrasound, or MRI — will be necessary. If an abnormality is identified with breast imaging, then a needle biopsy will be performed. In a needle biopsy, a thin, hollow needle is used to extract a sample that can be examined under a microscope. If an abnormality is not identified with breast imaging, then a punch biopsy of the skin can be performed. During a punch biopsy, a special tool that looks kind of like a miniature cookie cutter is used to take a sample of all the layers of skin. Local anesthetic is used to numb the area before the procedure so you won’t feel pain during the biopsy.
Because IBC can be difficult to diagnose and because it is typically a more aggressive form of breast cancer, the cancer may have spread outside of the breast by the time it is found. Staging studies can be performed to look for cancer that has spread to other parts of the body.
How is inflammatory breast cancer treated?
IBC can grow quickly, so it’s necessary to start treatment immediately after diagnosis. The sooner treatment starts, the better the chances are of recovery.
Treatment for inflammatory breast cancer usually involves a combination of chemotherapy, surgery, and radiation. Chemotherapy is often given before surgery, and then surgery is performed to remove the affected breast tissue and lymph nodes. Radiation is delivered after surgery. Some types of IBC respond to hormone-lowering medications, so these may be given in addition to the other treatments. Lastly, some people may choose to participate in clinical trials to try out new treatments that aren’t widely available to the public yet.
When to see a health care provider about changes to the skin of the breast?
Even though breast skin changes usually don’t mean anything serious, it's important to know when you might actually need medical attention.
If wearing more breathable fabrics; avoiding soaps and detergents that cause skin sensitivity; and keeping your breasts clean and dry doesn’t seem to help with the skin changes you’re seeing, or if you notice your symptoms worsening, be sure to check in with a health care provider. And be sure to visit a health care provider if you notice any of these accompanying symptoms:
- Pain
- Fever
- Sores
- Unusual (green or yellow) or foul-smelling fluid coming from the inflamed area
Although IBC is rare, being vigilant about breast health saves lives, so be sure to keep these symptoms in mind. If you have any concerns about changes in your breast tissue or skin of the breast that can’t be easily explained, it’s essential to see a health care provider.
Rashes that don’t go away by themselves may need medical treatment even if they’re not a serious threat, so don’t hesitate to ask for some professional advice.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.

