Want to find out more about the effects of birth control on the female body? Read the first part of our exclusive interview with Professor Johannes Bitzer, former president of the European Society of Contraception and one of the leading experts in the field of birth control.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
The Effects of Birth Control: An Interview with Professor Johannes Bitzer, Part 1

Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
This is the first part of our two-part interview with Professor Johannes Bitzer. The second part of the interview can be found here.
Which contraception methods have the least side effects?
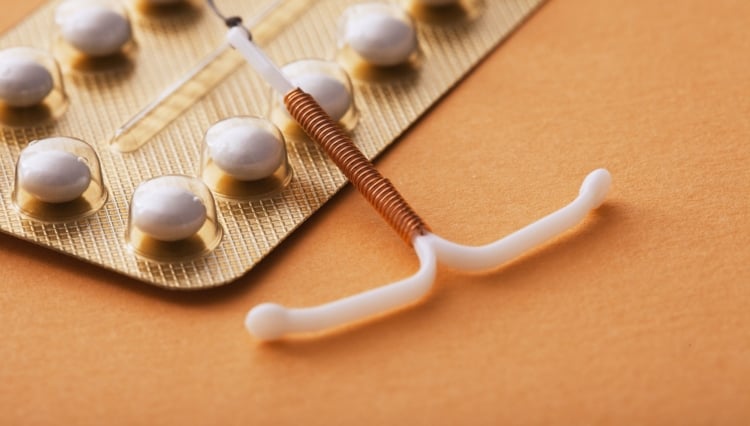
“If you look at just possible health risks and side effects, we could say that one of the least ‘risky’ methods is probably the copper IUD,” Professor Bitzer says.
It doesn’t have a negative impact on metabolism or the cardiovascular system. If you place it properly, there are no major gynecological complications. Taking the very broad view, the copper IUD has a very good risk-to-benefit profile.
“The most complicated issue is actually with hormonal contraception,” adds Johannes Bitzer, who further explains that there are two basic types of hormonal birth control pills. One is combined hormonal contraceptives, which contain progestogen and estrogen. The other group only contains progestogen.
All the combined oral contraceptives (COCs) have a cardiovascular risk, especially of venous thrombosis. The risk is low, but it can be a dangerous complication. Fortunately, it’s very rare, but the risk is there, and it increases when you take COCs.
If you take hormonal contraceptives without estrogen, you don’t have this thromboembolic risk. So progestogen-only contraception also has a favorable benefit/risk profile. Moreover, progestogens can be taken as pills, implants, and intrauterine systems.
Professor Bitzer explains that with birth control, it’s more of a tolerability issue. The side effects you might have aren’t dangerous, but can be rather uncomfortable, especially those regarding bleeding irregularities. And here the combined oral contraceptives have additional benefits: they regulate the cycle, are good for your skin, and protect against certain health conditions.
All in all, COCs present the most complicated picture: They have benefits, but there are also risks. On the general level, the copper IUD is probably the birth control with the least risk, followed by progestogen-only contraceptives.

Take a quiz
Find out what you can do with our Health Assistant
Which birth control methods are the most effective?
“Many studies have shown that the most effective methods are these long-acting methods we’ve been talking about, namely IUDs and hormonal implants. They are almost 100 percent effective. Nothing is exactly 100 percent, but they are close — around 99.5 percent,” says Professor Bitzer.
He also adds that other methods like the pill would also be similarly effective, but not with what we call typical use: “You need to take the pill every day, and people have difficulty sticking to the schedule.”
So if you want maximum effectiveness with minimum hassle, long-lasting birth control methods are best.
What happens if you miss a week of birth control pills?
When you forget your pill matters. Johannes Bitzer says of all the times to miss a pill, forgetting to take it after the seven-day break creates the greatest risk of pregnancy. Most people still take the classic pill with 21 days of active pills, followed by a seven-day break or seven days of placebo pills. Forgetting the pill within the first week after the break creates such a high risk of pregnancy because follicles in the ovaries started growing during the break. When they’re not suppressed by regular intake in that first week, breakthrough ovulation occurs.
“So when you forget one or even two pills during the first week, you need to take emergency contraception because you’re not protected very well anymore,” says Professor Bitzer. “If you forget one or even two pills in the middle of your package, just take the pills you forgot later. This is not so risky, because you have seven days of regular intake, which is good for the suppression of the ovaries. These are the general rules. When you are not secure, you need to use emergency contraception in addition to your pill.” And using condoms is also an option.
Can birth control make breasts bigger?
Regarding breasts getting bigger because of birth control, Professor Bitzer says that what sometimes happens, especially when people first start taking birth control, is the estrogen component in the pill causes some water retention. “This is not really breast growth, it is more of water retention inside the glands, the tissue.”
Can birth control pills cause breast rashes?
According to Professor Bitzer, rashes are rare. They don’t usually have anything to do with the pill. Often, they’re just coincidental. There are rare occasions when the body reacts to the progestogen in the pill, especially after exposure to sunlight. This could cause skin coloration. It is rare, but that is a consequence of the pill.
Can birth control pills treat Polycystic Ovary Syndrome?
According to Professor Bitzer, “Yes, they can help treat the symptoms of PCOS. They cannot heal PCOS, but we can quite effectively treat the symptoms.”
He also says that the most important symptoms to treat are cycle irregularity, heavier bleeding, acne, and hirsutism. They can be very effectively treated with birth control pills, especially pills that contain anti-androgenic progestins. These progestins counteract the effect of testosterone to effectively treat the symptoms.
Read this next: a detailed interview about PCOS with Professor Tahir Mahmood

Does taking the pill for a long time affect the cycle?
Professor Bitzer says that this has been studied very extensively out of concern for people who start taking the pill when they’re very young and continue taking it for 20 years. Researchers wanted to know if they develop problems with their cycle or fertility. In fact, some people don’t get periods after they stop taking the pill. This is called amenorrhea. However, studies have shown that people who experience this actually had this problem before they started taking the pill, but they didn’t realize it because taking the pill gave them regular bleeding. “The pill itself doesn’t cause endocrine problems, but the endocrine problems may appear after stopping the pill,” explains Professor Bitzer.
Classic endocrine problems are PCOS or hypothalamic amenorrhea — for people who take hormonal birth control, they’re often not detected until they stop taking it.
Can you lose fertility after taking the pill for years?
According to Professor Bitzer, “It has become very clear that pill use protects fertility. You get less infection, fewer ectopic pregnancies, of course. Regarding fertility, you’re better off using the pill than not.”
How long should you wait to get pregnant after reversible contraception?
Professor Bitzer says you don’t need to wait: There isn’t a negative long-term effect. You just get off the contraceptives and get pregnant.
Can birth control pills cause strokes or aneurysms?
According to Professor Bitzer, we should be careful when talking about the cause of these serious conditions, because they’re usually caused by a combination of factors. The birth control pill is a risk factor.
Says Bitzer, “There is some association between the pills and stroke — a very low risk, but there is some association. There is no association with aneurysm. An aneurysm is something inborn, it has nothing to do with the pill. So, the important issues are venous thrombosis and arterial complications like myocardial infarction or stroke. They are very rare, but if you take a sample size of hundreds and thousands of women, there is some association.”
How can birth control weight gain be avoided?
“In general, there is no clear scientific evidence of weight gain,” says Professor Bitzer.
He further explains that there have been a lot of studies comparing birth control users with non-users or IUD users for six months or even a year, and in all the groups, women gain weight: “We don’t know why, but the studies didn’t find a difference. In clinical practice, I think there are some women who really experience the anabolic effect of the progestogen, and I have to believe them. And I believe that they feel they gained weight. But probably, there are very few cases where it is really the pill that makes them gain weight.”
Is spotting while taking birth control pills normal?
Spotting is normal during the first three months and even later in the sense that it’s not a sign of a disease, says Professor Bitzer: “But what happens is that you give these hormones externally and the mucosa in the uterus has to adapt to these hormones. You give both hormones every day, which is different from the natural cycle. This may lead to the fact that the endometrium has a little breakthrough bleeding, some spotting.”
It’s not a disease, it’s not dangerous. It usually disappears, but it also may come back a little bit later. The professor says that it’s not something to be worried about.
What are birth control contraindications?
There are contraindications for each method. Professor Bitzer says that if you’re considering combined hormonal methods ( the pill, patch, or vaginal ring), the main contraindications are connected to the risk of thrombosis: family history or personal history of thrombosis and also specific genetic issues, like thrombophilia, for instance.
According to the professor, “There are age-related issues. Women after 40 need to be very careful with combined oral contraceptives when they are overweight and smoke more than 15 cigarettes a day.”
He says there are also some false beliefs about contraindications — “Having breast cancer in the family, for instance, is not a contraindication. Although having breast cancer already is a contraindication.”
For progestogen-only contraceptives, he says there are almost no contraindications (only specific rare diseases and some cancers).
For the copper and the hormonal IUDs, the only contraindication is bleeding when you don’t know where it comes from or acute infection of the uterus.
He also says, “For men, there is nothing known, really. Men are less in danger with their birth control options.”
What are some ways to stop worrying about birth control failing?
Professor Bitzer suggests that one of the important things is to be informed in a way that gives you confidence about the methods you use.
He says, “I think with all the studies and science, we can show that the birth control methods we’ve been talking about really protect against pregnancy so that you can rely on them and enjoy sexuality without having the fear of getting pregnant. I also think the fact that women talk with each other and inform each other and those who use these effective methods very rarely tell other women, ‘I had a failure.’”
What are popular misconceptions about birth control?
Professor Bitzer says hormones are a big one: “It’s important to learn about the hormones used for contraception. Many people believe the hormones are dangerous, almost like a chemical poison.”
But this is not the reality, as he further explains. “The hormones used in birth control are actually equivalents to the body’s hormones. It’s a sort of body language. What we are trying to do is to give signals to the body that you don’t need to reproduce because you are already pregnant. It’s like a low-level pregnancy.”
He says that in the last 60–70 years we have collected a lot of information about birth control pills, and we can now state — and this is general agreement all over the world, including medical authorities — that the benefit of hormonal contraception is much higher than the risk.
According to the professor, the biggest benefit of birth control is an effective protection against pregnancy: “Pregnancy can be very dangerous. Hormonal contraceptives protect against ovarian and endometrial cancer; they’re good for osteoporosis; they treat endometriosis pain, dysmenorrhea, and algomenorrhea. They’re good for the skin — a whole list of good things.”
He continues, “We also, of course, know about risks. We know that there is a small increase in thromboembolic risk — you might get a blood clot. But this refers to about three to four women per 10,000 cases, and this usually occurs right during the first year of use. We have become better at detecting those women who have additional risks and discouraging them from taking the pill. We are looking into family history, blood thrombophilia, and other risk factors. We also have to exclude women who are overweight or who smoke too much.
A big discussion is about breast cancer — women are concerned about it. It looks like there is a small increase in breast cancer risk while taking the pill in women of reproductive age. But the basic knowledge that we have now is that the pill itself doesn’t cause breast cancer, but in those women where breast cancer is developing, these hormones may accelerate it. It is also important to note that the risk is not lifelong. When you stop, it goes back to basic risk.”
In the end, when you take the pill there is a small risk of thromboembolic complications and even a smaller risk of breast cancer. “They’re real, but for the large majority (for 99,990 out of 100,000 women), hormonal contraceptives are safe,” concludes Professor Bitzer.
Don’t forget to check out the second part of our interview with Professor Johannes Bitzer here.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.




