There are several different types of cervical cancer, some of which are more common than others. The type usually depends on where in the cervix the cancer originates and if it spreads. When cervical cancer is detected early on with a Pap smear, it’s much easier to treat and has a better prognosis. Keep reading to learn all about the various types of cervical cancer, plus treatment and prevention to help keep yourself safe.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Types of Cervical Cancer: Essential Features to Know

Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
Anatomy of the cervix
The cervix has a few different components. The endocervix is the opening leading into the uterus. Below that is the exocervix, which is just above the vagina. The exocervix is what the OB-GYN sees during an exam. These regions meet at what’s known as the transformation zone, which is the place where most cervical cancers begin. Take a look at the image below to get a better understanding of where these are located within the reproductive system:
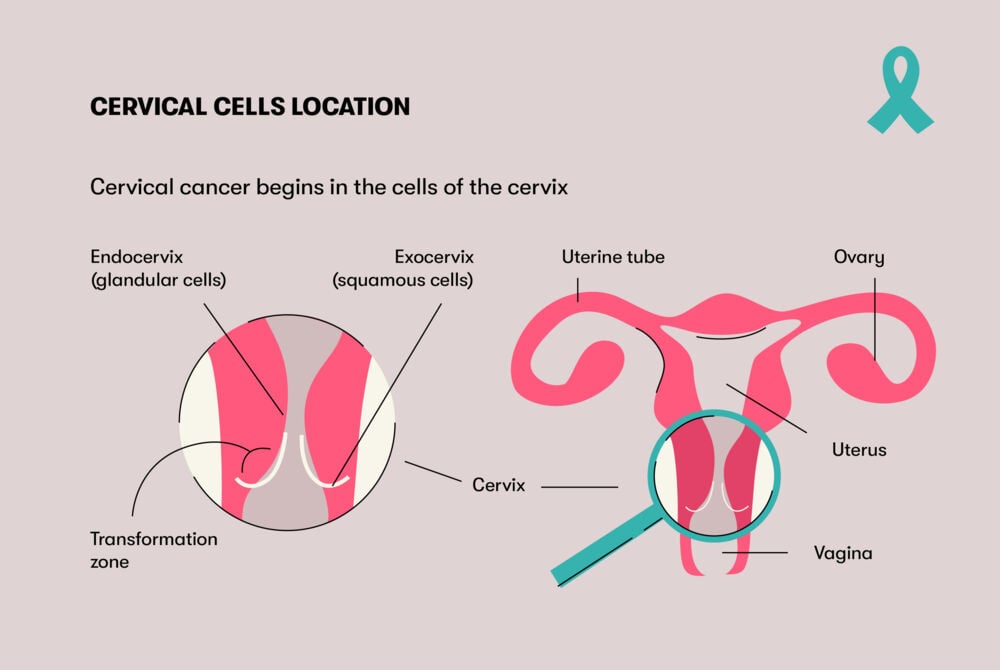
Common types of cervical cancer
Cervical cells don’t just suddenly become cancer. Rather, it’s a slow process as the cells go through some abnormal changes, known as precancer, which may eventually develop into cancer if left untreated. There are two main common types of cervical cancer, plus a third type that’s a combination of the other two. The types are classified according to how they look in a lab under a microscope.
Squamous cell carcinoma
Squamous cell carcinomas account for around 70 percent of cervical cancers, according to the SEER Cancer Statistics Review. Most squamous cell carcinomas begin in the cells near the transformation zone (where the exocervix and endocervix meet).
Adenocarcinoma
Most other cervical cancers are adenocarcinomas, or endocervical adenocarcinomas. These develop from the glandular cells that produce mucus.
They usually begin as a non-invasive type of cancer called adenocarcinoma in situ (AIS). AIS describes cancerous cells that only appear in one place.
Adenosquamous carcinoma
Some cervical cancers affect both squamous cells (in the transformation zone) and glandular cells (the ones that produce mucus) from the start. These are known as adenosquamous carcinomas or mixed carcinomas.
Rare types of cervical cancer
Besides these most common types, there are a few rarer types of cervical cancer, including metastatic cervical cancer, which is cancer that has spread significantly (i.e., metastasized) around the body. Other less-common types of cancer that can affect the cervix and other areas of the body include:
- Sarcoma
- Lymphoma
- Small cell cervical cancer
Early diagnosis saves lives
Many people with cervical cancer don’t notice any signs early on, because symptoms generally appear when the cancer progresses to a later stage. This is why it’s so important to have regular gynecological checkups that look for changes in the cervix that could develop into cancer. These checkups can detect cervical cancer while it’s still at a very early stage, when there’s a better prognosis for recovery.
These are the symptoms of cervical cancer to be aware of:
- Periods that are much heavier or last longer than usual
- Unexpected vaginal bleeding and bleeding after sex
- Lower abdominal, low back, or pelvic pain
- Unusual vaginal discharge
After a cervical cancer diagnosis, an oncology team — a group of medical professionals who specialize in cancer treatments — may order tests to check whether the cancer has spread anywhere else in the body (known as invasive carcinoma). After that, the team will create a personalized action plan for treatment to target all of the affected areas.
Treatments can include surgery to remove the cancerous cells, as well as chemotherapy (cycles of medication) or radiotherapy (x-rays) to reduce the number of affected cells or treat other parts of the body. Health care providers may combine treatments depending on the particular case to boost the effectiveness. The good news is that when cervical cancer is caught early enough (with a Pap smear), it’s very treatable.
In fact, cervical cancer used to be the highest cause of cancer death for American women, but the U.S. National Cancer Institute reports that deaths have decreased by 75 percent since the 1950s, thanks to advances in screening and treatment techniques.
Keep these symptoms in mind and stay in tune with your body so you’ll know if something doesn’t feel right. Don’t hesitate to reach out to a health care provider if you have any questions or concerns about cervical cancer, and remember to get regular pelvic exams and Pap smears at the OB-GYN to protect your health.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.

