Characterized by a gradual reduction in fetal heart rate (FHR) patterns that is visually detectable, late decelerations warrant a closer look. Together with Flo, learn more about the contributing factors of late decelerations and proven methods of treatment.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Late Decelerations: What They Mean and How to Manage Them


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
What are late decelerations?
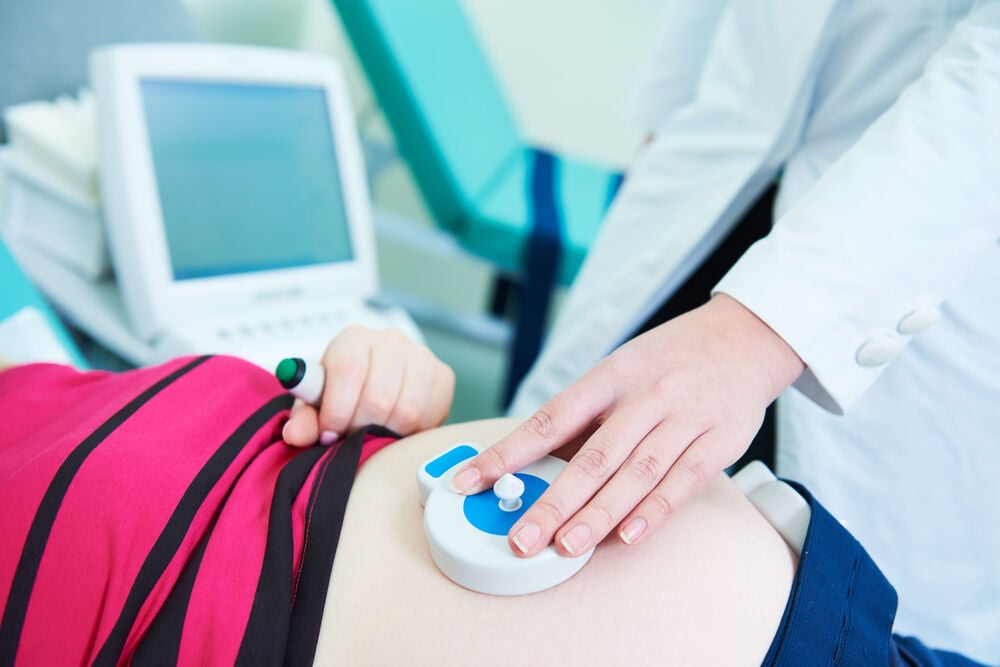
Fetal heart rate is a vital indicator of your baby’s health. Your doctor checks the status during labor and delivery by monitoring and measuring their heart rate using special equipment. This detects changes in the normal FHR pattern at the time of labor, reassuring your obstetrician if it’s safe to proceed.
Believed to be an abnormal FHR pattern, late decelerations indicate a reduction in heart rate, usually after a uterine contraction. Once deceleration starts, it takes about 20 to 30 seconds to reach its lowest point. When the timing of deceleration is delayed, it means that the lowest point is occurring past the peak of your uterine contraction.
In the majority of cases, the beginning, low point, and recovery of late decelerations happen after the start, peak, and end of your contraction, respectively.
One of many unusual FHR patterns observed during labor, late decelerations could be considered dangerous. They’re a sign of hampered blood flow to your placenta, which might trigger imminent fetal hypoxia (or a lack of oxygen for fetal tissues).
Are late decelerations a cause for concern?
Take a quiz
Find out what you can do with our Health Assistant
While late decelerations sometimes point to an abnormally low concentration of fetal blood oxygen (i.e., fetal hypoxemia), various other factors could be at play. Medications you’ve taken, as well as gestational age could impact FHR patterns.
As such, fetal heart tracings should be combined with other clinical methods to ensure accurate interpretation of your baby’s condition. It’s unlikely that your fetus is receiving insufficient oxygen to centrally located organs if they’re sustaining a stable baseline heart rate with a reassuring variability.
While late decelerations sometimes point to an abnormally low concentration of fetal blood oxygen, various other factors could be at play.
However, when late decels occur in more than 50 percent of the contractions of your uterus, then fetal hypoxia is a plausible explanation. Your doctor will then take action to prevent medical complications for your newborn.
Causes of late decelerations
Uterine contractions compress the blood vessels present in your uterine wall, reducing blood flow to your placenta. This could temporarily restrict your fetus’ oxygen supply.
Your doctor should be on the lookout for late decelerations which occur in association with tachycardia (i.e., a fast heart rate) and much less variability. They might represent the harmful effects of uterine contractions.
Furthermore, chronic dysfunction of your placenta is sometimes brought on by maternal diseases, like diabetes, collagen-vascular disorders, or hypertension.
Usually, any process that causes the following conditions is capable of inducing late decelerations:
- Maternal low blood pressure (or hypotension)
- Excessive activity in your uterus
- Reduced oxygen supply to your placenta
Two of the most common late deceleration causes include an overactive uterus and hypotension due to epidural analgesia. This is the injection of an anesthetic into your spinal epidural space to eliminate pelvic pain during labor and delivery.
Furthermore, chronic dysfunction of your placenta is sometimes brought on by maternal diseases, like diabetes, collagen-vascular disorders, or hypertension. Lastly, late decelerations and fetal hypoxia during the second stage of labor could be the result of your pushing.
Late decelerations treatment and management
If the fetal heart rate pattern is atypical, then your obstetrician will initially try to determine the underlying problem. Diagnosis of this condition requires clinical acumen to know whether these problems are reversible or not. When they suspect fetal hypoxia, they must determine the delivery timing to prevent serious consequences for your newborn. That said, they should also attempt to avoid delivering your baby unnecessarily early.
The chances of fetal hypoxia remain low if repeated decelerations aren’t present and fetal heart tracing is otherwise normal.
It’s essential to evaluate complete fetal heart tracings, along with the status of your own health. Additionally, your doctor should check for the absence/presence of decelerations, degree of variability, and immediately address the root cause of late decelerations. Keep in mind this doesn’t mean you’ll need an instrumental vaginal or cesarean delivery right away.
The International Federation of Gynecology and Obstetrics (FIGO) released specific guidelines on the subject. They’ve concluded that the chances of fetal hypoxia remain low if repeated decelerations aren’t present and fetal heart tracing is otherwise normal.
When a doctor suspects fetal hypoxia, they must determine the delivery timing to prevent serious consequences for your newborn.
If your doctor identifies reversible causes, they’ll likely conduct other tests and closely monitor you. Also, you can take certain steps to treat late decelerations and improve fetal oxygen supply.
- Lie down in the left lateral, knee-chest, or right lateral position to relieve compression of the large vein (or vena cava) by your pregnant uterus. This increases the flow of deoxygenated blood to your heart and body, including your uterus and placenta.
- Your doctor might administer oxygen in response to late decelerations. However, there’s no clinical evidence suggesting its effectiveness when used alone in women with adequate oxygen levels.
- If you develop hypotension after spinal or epidural analgesia, they may choose to administer fluid at the time of labor. Similarly, clinical research doesn’t support its efficacy in individuals with normal blood pressure.
- Your doctor might ask you to stop pushing efforts, which causes fetal hypoxia to progress rapidly, in the second stage of labor.
If the above steps don’t prove useful in dealing with late decelerations, especially when they recur and last more than 30 minutes, delivery is a wise option. This would also be the case if other tests indicate any issues with your baby. When this happens, a prompt C-section is normally the method of choice.
Possible complications of late decelerations
Complications arising from repeated or prolonged late decelerations include:
- A low APGAR (i.e., appearance, pulse, grimace, activity, and respiration) score
- Greater chance of admission to the neonatal intensive care unit after delivery
- Cerebral palsy
- Neonatal encephalopathy
Takeaway
A multidisciplinary team of health care professionals manages the process of labor and delivery for you. If FHR monitoring shows late decelerations, it’s critical to further evaluate complete fetal heart tracing results and take swift action.
In order to prevent severe brain injury from a lack of oxygen, your doctor must revive the fetus and quickly address the source of late decels. In the absence of improvement, immediate delivery is a strong possibility. Rest assured, however, that babies who receive prompt treatment have an excellent outcome.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
History of updates
Current version (04 November 2020)
Published (30 December 2019)
In this article
Get your personal guide to pregnancy with the Flo app
-
Follow your baby's growth week by week
-
Get expert info on symptoms, safe foods, and more
-
Chat with other parents-to-be




