Thinking about getting the COVID-19 vaccine or booster shots during pregnancy? Flo has rounded up the latest information here to help you make an informed decision.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
COVID vaccine during pregnancy: Everything you need to know


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
Adding to your family at any time can bring up lots of questions and considerations. If you’re having a baby during the coronavirus pandemic, you may have some specific concerns about potential health risks to you and your baby if you catch COVID or want to get the COVID vaccine. That’s why we’ve pulled together this guide.
Before we jump into the facts around getting the COVID vaccine during pregnancy, you might be wondering what the impact of COVID is on those of us who are pregnant. The truth is there isn’t any evidence that shows that being pregnant increases your risk of catching COVID-19. But what we do know is if someone who is pregnant catches COVID, they have a higher risk of being hospitalized and needing intensive care.
A study published in the BMC Pregnancy and Childbirth journal in April 2021 looked into the risk of severe illness between pregnant and non-pregnant women. Researchers found that compared to those who weren’t expecting, pregnant women had much higher rates of needing to go to the hospital due to their symptoms (60.5% vs. 17%).
If you’re pregnant and get COVID (especially if you get severely ill), there’s also a greater risk of preterm birth and other pregnancy complications, according to a January 2021 study conducted by the US National Institutes of Health. And, although rare, it’s also possible for a pregnant person to transfer COVID-19 to their baby.
As for those who are breastfeeding, it’s thought that their risk of serious illness from COVID is the same as for those who aren’t pregnant.
Now that we know the potential risks to pregnant people and babies when it comes to COVID infection, let’s see what the experts have to say about getting the COVID-19 vaccine while pregnant.

COVID vaccine during pregnancy: Is it safe?
Chances are you know that everything you put into your body during pregnancy goes to your baby too. So you may have some questions about whether or not COVID vaccination during pregnancy is safe for both of you.
It may help to know that the Centers for Disease Control and Prevention (CDC), American College of Obstetricians and Gynecologists, American Society for Reproductive Medicine, and the Society for Maternal-Fetal Medicine all agree that COVID vaccines should be offered to pregnant people.
The European Board & College of Obstetrics and Gynecology believes that vaccination against COVID during pregnancy should be offered to any pregnant person who wants it.
Evidence continues to build showing that COVID-19 vaccination during pregnancy is safe and effective. Getting vaccinated will allow your body to build immunity while reducing your risk of getting very sick with COVID-19 and having any coronavirus-related pregnancy complications. The World Health Organization doesn’t believe there are any risks for pregnant people that outweigh the benefits of getting vaccinated.
When should you get the COVID-19 vaccine during pregnancy?
The CDC and professional medical organizations, including the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine, recommend COVID-19 vaccination at any point in pregnancy, as well as booster doses for those who are eligible.
Vaccination can protect you from getting very sick from COVID, and keeping you as healthy as possible during pregnancy is important for the health of your baby.
When it comes to research, the CDC and Food and Drug Administration haven’t found any safety concerns for vaccinated pregnant people or their babies. There also haven’t been any miscarriages, stillbirths, or preterm births linked to the vaccines, nor is there any evidence that the COVID-19 vaccines cause fertility issues, so you don’t need to be concerned if you plan to get pregnant later on.
In short, getting vaccinated has fewer risks than getting COVID-19, especially for pregnant people. But getting vaccinated is everyone’s personal choice, and you get to decide if it’s the right move for you during pregnancy.
Take a quiz
Find out what you can do with our Health Assistant
Which COVID vaccine is safe during pregnancy?
Numerous COVID-19 vaccines have been developed worldwide, falling into four different categories:
- Whole virus: exposes the body to a weakened or dead form of the COVID-19 virus to build immunity
- Protein subunit: uses specific parts of the COVID-19 virus to trigger the immune system (mRNA vaccines like Pfizer-BioNTech and Moderna)
- Viral vector: gives the body instructions to fight COVID-19 using a harmless virus (vaccines like AstraZeneca and Johnson & Johnson)
- Nucleic acid (RNA or DNA): tells the body how to fight COVID-19 using genes
Experts recommend the Pfizer or Moderna mRNA vaccines for those who are pregnant if available because data hasn’t shown any safety concerns for pregnant people with these vaccines.
In fact, an April 2021 study of 35,691 pregnant women aged 16–54 looked into the safety of COVID-19 vaccination during pregnancy and didn’t find any issues with the mRNA vaccines (Pfizer or Moderna). There were also studies conducted on animals that received COVID vaccines before or during pregnancy that didn’t find any safety issues for the pregnant animals or their babies.
Because the vaccines don’t contain live viruses (at least the ones authorized for use in the United States and European Union), they can’t give you or your baby COVID.
In fact, COVID vaccination while pregnant may even help protect babies from getting COVID-19 after they’re born. Recent reports have shown that pregnant women and people (mostly in the third trimester) who received mRNA vaccines passed the antibodies down to their babies, so they both built immunity.
Different vaccines are approved and available depending on where you live, so it’s best to check the following websites for the latest local information:
If you’re pregnant and thinking about getting vaccinated, experts recommend discussing it with your health care provider. You can also ask which vaccines are offered at your doctor’s office or vaccination location.
Should I get the COVID vaccine while breastfeeding?
You may wonder about the timing of your vaccination once you start breastfeeding. What if you get the first dose of vaccine while you’re still pregnant and then the second one after you deliver?
You might find it helpful to know that according to experts, based on how vaccines work in the body, there shouldn’t be any risk to you or your baby in this case. Doctors from Johns Hopkins Medicine have stated that if you get vaccinated, there’s no need to stop breastfeeding.
A March 2021 study of 131 participants (84 pregnant, 31 lactating, and 16 non-pregnant women) confirmed that vaccination doesn’t pose a health risk to the mother or the baby (both while pregnant and while breastfeeding). It also found that lactating parents who receive the mRNA vaccines pass antibodies down to their babies through their breast milk, which can help protect the baby.
COVID vaccine during pregnancy: When do you gain immunity after getting vaccinated?
It takes around two weeks for the body to build immunity after receiving the full dosage of the vaccine. As this is such a new topic, researchers are still learning how long COVID-19 vaccine protection lasts.
COVID vaccine during pregnancy: What are the possible side effects?
It’s possible to feel some side effects after COVID-19 vaccination, including:
- Tiredness
- Headache
- Chills
- Fever
- Pain or tenderness in the arm where you got the shot
These are normal signals that your body is building immunity to the virus, and they should go away within a few days.
There is one more side effect that is extremely rare but worth mentioning: blood clots following vaccination. While authorities believe that benefits outweigh possible harm, it’s up to you to decide if you’re OK with the risks.
And finally, it’s important to note that it’s not possible to catch COVID-19 from the vaccine.
How does COVID vaccination work during pregnancy?
Getting the COVID vaccine during pregnancy is the same as for people who aren’t pregnant (via a shot in the arm administered in one or two doses).
The Pfizer, Moderna, and AstraZeneca vaccines need two shots to build immunity, while the Johnson & Johnson vaccine is only one shot. It’s now advised that the second shot be the same vaccine as the first one you got.
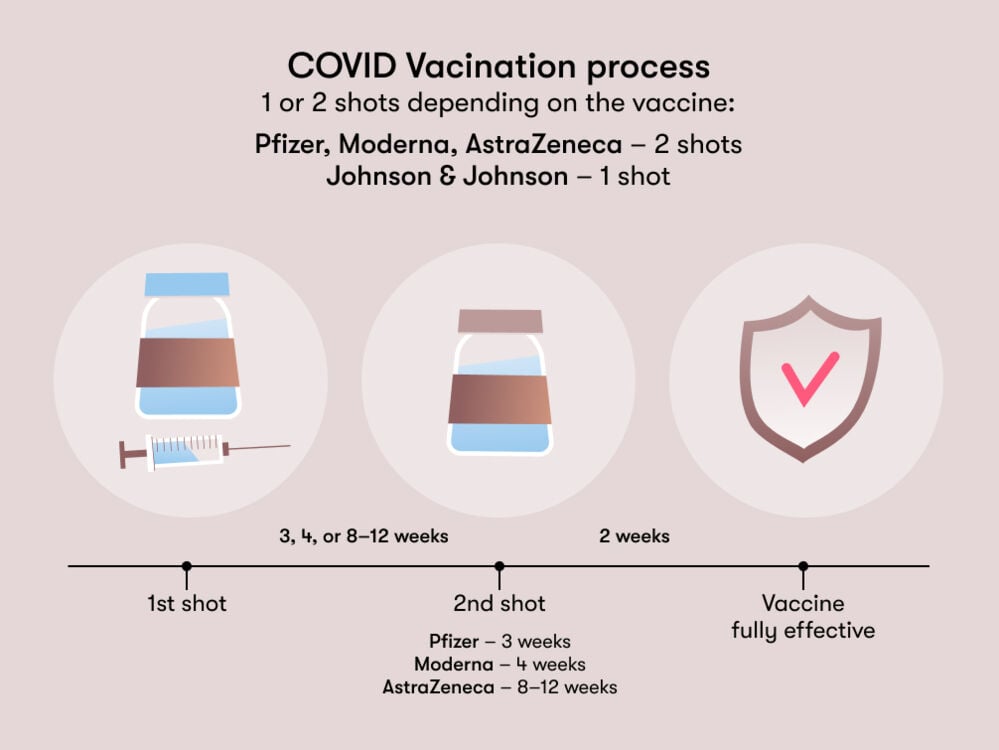
But sometimes it’s necessary to take doses from different vaccines, like if the first dose of a specific vaccine prompts a severe allergic reaction or if there is a shortage of the same vaccine locally. Some studies, including research by the University of Oxford in June 2021, have found that mixing vaccines might even boost the immune response, but the safety and effectiveness of mixing different vaccines are still being explored.
Usually, a second dose of the Pfizer vaccine is recommended three weeks (21 days) after the first one; the Moderna vaccine’s second dose is recommended four weeks (28 days) later; and the second dose of the AstraZeneca vaccine is given between 8 and 12 weeks (56–84 days) afterward. But local regulations might differ where you are, so it’s a good idea to check.
It takes two weeks after the final shot to get the full effectiveness of the vaccine. This is the point when you’re considered fully vaccinated.
COVID vaccine during pregnancy: How to prepare to get your shot
Leading up to your vaccination, it’s not recommended to avoid, stop, or delay medications for any other health conditions, but be sure to always check your medication with your health care provider if you’re pregnant or breastfeeding.
The CDC also doesn’t recommend taking over-the-counter medicine or pain or allergy medication before you get vaccinated to try to prevent side effects. Researchers don’t know what impact they have on the vaccine’s effectiveness. Other than that, there’s nothing special that you need to do to prepare.
COVID vaccine during pregnancy: The takeaway
Experts say that the COVID-19 vaccines are our best hope of ending this pandemic. Data on the impact of COVID vaccination while pregnant or breastfeeding is growing, and so far there isn’t any evidence to suggest it poses any health risks. In fact, recent studies have confirmed this.
Nevertheless, it’s important to consult a health care provider about the risks of acquiring COVID-19 infection in pregnancy and the existing evidence on the benefits and potential side effects of vaccines. Researchers are learning more about COVID and vaccines all the time, so information can change quickly. Ask your doctor or health care professional if you have any questions.
Remember that being vaccinated doesn’t mean you’re 100% immune from catching COVID, but if you get it, your risks of getting very sick are lower. If you do end up with COVID even though you’re vaccinated, you can still pass it to others, so continue following local guidelines around social distancing, mask wearing, and hand washing to prevent catching and spreading it.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
“COVID-19 Vaccines While Pregnant or Breastfeeding.” Centers for Disease Control and Prevention. 18 Mar. 2022, https://www.cdc.gov/coronavirus/2019-ncov/vaccines/recommendations/pregnancy.html.
“Key Things to Know.” Centers for Disease Control and Prevention, 12 May 2021, https://www.cdc.gov/coronavirus/2019-ncov/vaccines/keythingstoknow.html#:~:text=It%20typically%20takes%20two%20weeks,after%20a%20one%2Ddose%20vaccine.
Goldfarb, Ilona T. “Wondering about COVID-19 Vaccines if You’re Pregnant or Considering Pregnancy?” Harvard Health Publishing, 7 Jan. 2021, https://www.health.harvard.edu/blog/wondering-about-covid-19-vaccines-if-youre-pregnant-or-breastfeeding-2021010721722
Sheffield, Jeanne and Andrew Satin. “The COVID-19 Vaccine and Pregnancy: What You Need to Know.” Johns Hopkins Medicine, 9 Feb. 2021, https://www.hopkinsmedicine.org/health/conditions-and-diseases/coronavirus/the-covid19-vaccine-and-pregnancy-what-you-need-to-know
“Preparing for Your Vaccine.” Centers for Disease Control and Prevention, 19 Apr. 2021, https://www.cdc.gov/coronavirus/2019-ncov/vaccines/prepare-for-vaccination.html
“If You Need a Second Shot.” Centers for Disease Control and Prevention, 27 Apr. 2021, https://www.cdc.gov/coronavirus/2019-ncov/vaccines/second-shot.html
Bianchi, Diana W. “Severe COVID-19 in Pregnancy Associated with Preterm Birth, and Other Complications.” National Institutes of Health, US Department of Health and Human Services, 28 Jan. 2021, https://www.nih.gov/news-events/news-releases/severe-covid-19-pregnancy-associated-preterm-birth-other-complications
“COVID-19 Vaccines: Get the Facts.” Mayo Clinic, 15 May 2021, https://www.mayoclinic.org/coronavirus-vaccine/art-20484859#pregnant-breastfeeding
Shimabukuro, Tom T., et al. “Preliminary Findings of mRNA Covid-19 Vaccine Safety in Pregnant Persons.” The New England Journal of Medicine, vol. 384, 17 Jun. 2021, pp. 2273–2282, DOI: 10.1056/NEJMoa2104983, https://www.nejm.org/doi/full/10.1056/NEJMoa2104983
“Is It Safe to Get the COVID-19 Vaccine If You’re Pregnant?” Cleveland Clinic, 19 Apr. 2021, https://health.clevelandclinic.org/is-it-safe-to-get-the-covid-19-vaccine-if-youre-pregnant/
Gray, Kathryn J., et al. “Coronavirus Disease 2019 Vaccine Response in Pregnant and Lactating Women: A Cohort Study.” American Journal of Obstetrics & Gynecology, vol. 22, no. 303, Sep. 2021, pp. e1–17, https://www.ajog.org/article/S0002-9378(21)00187-3/pdf
“Covid-19 Vaccines, Pregnancy and Breastfeeding.” Royal College of Obstetricians & Gynaecologists, 14 May 2021, https://www.rcog.org.uk/en/guidelines-research-services/coronavirus-covid-19-pregnancy-and-womens-health/covid-19-vaccines-and-pregnancy/covid-19-vaccines-pregnancy-and-breastfeeding/
“Safe COVID-19 Vaccines for Europeans.” European Commission, 25 May 2021, https://ec.europa.eu/info/live-work-travel-eu/coronavirus-response/safe-covid-19-vaccines-europeans_en




