More people than ever before are thinking about preserving their fertility for the future. But what’s the difference between freezing eggs vs. embryos, and which is the best option for you? We asked an expert.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
What are the differences between freezing eggs vs. embryos?


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
If you’ve ever considered freezing your eggs or embryos for future family planning, then you’re not alone. It’s estimated that around one-third of all fertility treatments and procedures that took place in the US in 2019 were for patients who wanted to do just that.
The two procedures have given women and people who have periods more choice around when they have children and how they will conceive. But they’re also quite different (more on that below), and there’s a lot to consider, especially with the costs involved.
Here, Dr. Barbara Levy, Flo board member and clinical professor of obstetrics and gynecology, outlines exactly what happens when you choose to freeze your eggs vs. embryos and some of the questions you should consider asking your health care provider before you start treatment.
Freezing eggs vs. embryos: What’s the difference?
The process of choosing between freezing eggs or embryos can appear pretty confusing. However, there’s one big difference between the treatments.
When you freeze your eggs, they are unfertilized. We all know that when you’re trying to conceive, an egg represents 50% of the material required to make a baby — the sperm provides the other 50%. “An egg is not even a full cell — it’s a gamete,” says Dr. Levy. A gamete is the name given to the reproductive or sex cells (like an egg or sperm).
“It can’t function on its own,” says Dr. Levy. “It has half the number of chromosomes needed to make a baby. The sperm provides the other half.”
Take a quiz
Find out what you can do with our Health Assistant
An embryo is an egg that has been fertilized. “When an egg is fertilized by a sperm, it becomes a single cell,” says Dr. Levy. “Then, over the course of 3 or 4 days, the embryo divides several times. It goes from 1 to 2 to 4 to 8 cells, and so on.”
So how does the above information help you decide between freezing eggs or embryos? Well, there are two things to consider: your personal circumstances and the latest research.
If you don’t know who you want to have children with, then freezing your eggs may give you the freedom to start thinking about having a baby when you’ve met someone or are ready to pick a sperm donor. Alternatively, if you know you’d like to have children with a current partner but aren’t in a position to do so right away, then freezing embryos could be a better option.
Research has compared freezing eggs vs. embryos based on which treatment option is more likely to lead to babies being born. It can be difficult to identify exactly how many people freeze their eggs and then go on to have a baby, as there’s no guarantee that if someone freezes their eggs, they’ll go on to use them. Since egg freezing is no longer seen as an experimental procedure, the Human Fertilisation & Embryology Authority highlighted that it has massively increased in popularity, from just 230 cycles in 2009 to an estimated 2,400 in 2019.
The Human Fertilisation & Embryology Authority has noted that the odds of having a live birth from frozen eggs can vary depending on your age. Alternatively, the HFEA explained that due to development in fertility treatment and freezing technology, in vitro fertilization (IVF) treatments using frozen embryos have increased by 86% between 2014 and 2019.
Freezing eggs vs. embryos: How to prepare?
Before you get to the point of putting your eggs or embryos on ice, you need to stimulate the follicles in your ovaries to produce as many eggs as possible. Follicles are small sacs filled with fluid. Each ovary has around 8 to 15, and generally, each follicle has the ability to release an egg during ovulation.
To start this process, guided by your clinic, you will inject follicle-stimulating hormones (usually at night) for between 8 to 14 days. You’ll start around day 3 of your cycle.
A sonographer (medical professional who specializes in diagnostic images and scans) will then regularly check the size of your follicles. Your health care provider will also monitor your estrogen levels. They will do this through blood tests and an internal ultrasound. It’s important to remember here that there’s not a set number of eggs. We all respond differently to treatment, so try not to compare yourself to anyone else.
Once at least three of your follicles are big enough, around 18 mm, your health care provider will advise you to inject yourself with what’s called a “trigger shot” of a hormone known as human chorionic gonadotropin or hCG. This triggers the egg to mature and kickstarts ovulation. Around 36 hours later, your eggs will be collected in a process known as egg retrieval.
Feeling nervous about egg stimulation is completely understandable. But lots of people find they quickly get used to injecting the drugs. Natalie, who’s 35 and lives in London, had embryos frozen as part of IVF treatment. She says: “I was really worried about injecting myself, but using numbing cream on my tummy made it easier and less painful. My partner did the first couple of injections for me, and then I slowly started doing it myself each day. By the end of my treatment, injecting became a quick, easy, and pretty much pain-free part of my daily routine, even without the numbing cream.”
Speak to your clinic if you have any concerns. They’ll be able to share plenty of tips and advice.
Freezing eggs vs. embryos: How are eggs collected and fertilized?
So now that we know what happens during egg stimulation, let’s look at the next step: egg retrieval or collection.
This involves a small procedure while you’re under anesthetic. It takes as little as 20 minutes, and you will be sedated throughout. Your health care professional will use an internal vaginal ultrasound to get a proper look at your follicles. They will then use a suction device connected to a very thin needle to remove any eggs from the follicles. Not every follicle will contain an egg, but they will collect as many as they can.
Once you’re resting in the recovery room before going home, your doctor will let you know how many eggs they’ve collected. Experiencing a small amount of bleeding or cramping after the procedure is common, but if you’re at all concerned, then speak to your medical team. If you’re freezing your eggs, your clinic will then assess which eggs are mature (if the eggs are ready to be fertilized) and will freeze them promptly.
If you have decided to freeze embryos, then your eggs will be fertilized with sperm. Ahead of this, your health care provider will have spoken to you about whether you’re going to use your partner’s sperm, the sperm of someone you know, or a sperm donor, and a sample will have been provided.
The embryos will then grow for between 5 to 7 days under the careful watch of an embryologist, who will keep you updated on their progress. Some clinics may choose to freeze embryos slightly earlier (around day 3). Then they will be graded for quality before freezing. Not every embryo will make it to this stage, and that’s totally normal.
Whether you’re freezing your eggs or embryos, your period should arrive within two weeks after the egg collection, and your cycle should return to normal the following month.
How are embryos and eggs frozen?
Embryos and eggs are both frozen in the same way, which, in most clinics, is via a flash-freezing method known as vitrification. When an egg is vitrified, all biological processes, such as growing, will stop; this is why people refer to egg freezing as “freezing time.”
For freezing to work properly, eggs or embryos need to be cooled to -196 C (or -320 F). After egg collection and/or fertilization, lab technicians will put the cells into individual straws, carefully labeling them with a patient’s name and details, and then plunge them into liquid nitrogen, which cools the cells so fast that they freeze.
Special vitrification solutions (called cryoprotective agents) are used to protect your eggs or embryos from ice crystals in storage. All storage vessels should have temperature alarms, meaning that your clinic would be alerted if anything went wrong and your eggs or embryos warmed up during the storage process. You can speak to your health care provider about the storage they use before you go through with the freezing process.
Vitrification is a relatively new method of freezing eggs and embryos. Before it was developed, clinics would use a slower freezing method. Your health care provider would add a small amount of cryoprotective agent to your eggs or embryos. They would then be cooled slowly over two hours. After this, they would be stored in vessels of liquid nitrogen at -196 C (or -320 F).
Freezing embryos: Day 3 vs. day 5
While eggs are frozen within a day of being collected, embryos are given more time after being fertilized so they can develop.
Typically, embryos are either frozen around 3 days after they’ve been fertilized with sperm when they are six to eight cells or 5 to 7 days after fertilization when they’ve reached the blastocyst stage (between 50 and 200 cells). But which approach is best?
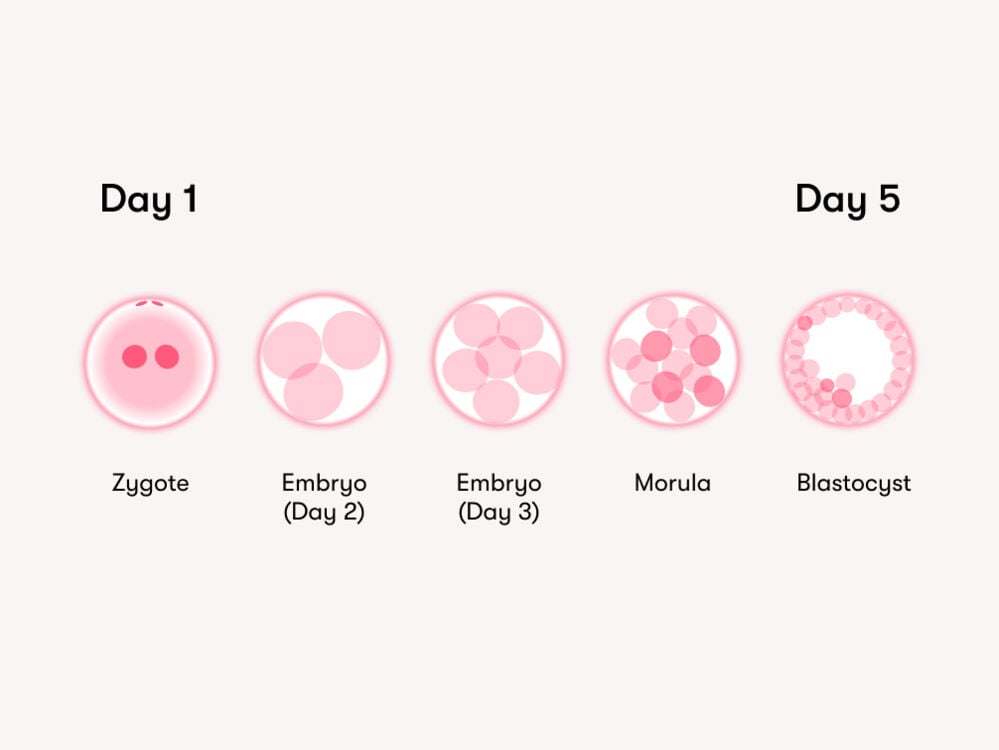
“The numbers are very clear,” says Dr. Levy. “When transferred to the uterus, day 5 embryos have a much higher success rate than day 3.” Yet every clinic will have a different perspective. Some will freeze good-quality embryos on day 3 because they believe the best place for the embryo to continue its development is in the uterus, and they worry they may not develop in the lab. Others work differently.
Talk to your health care provider to find out which approach your clinic uses and the science behind it.
Is it better to freeze eggs vs. embryos?
Like anything related to family planning, every person is different, so there’s no universal rule around the best approach to preserving fertility — you need to do what’s right for you.
Dr. Levy’s advice is to think about what your ideal outcome would be. Just like we discussed above, if you’re currently single, don’t know who you want to have children with, or are planning to explore using a sperm donor in the future, then freezing your eggs might be the best option for you. Alternatively, if you’d like to have children with a current partner at a later date, then freezing embryos might be a better option. Talking to a fertility specialist, along with friends and family, can help you make up your mind.
You may also want to consider how your fertility clinic will treat and eventually thaw your eggs and embryos. Research has looked at how eggs can be damaged during the thawing process.
“My understanding is that the surrounding structure of the tissue in an egg is more dense water and less ‘other fluid,’” explains Dr. Levy. “And so when you freeze an egg, it’s more likely to get ice crystals that are sharp and destroy it when you try to thaw it. Nowadays, we are better at thawing — but we have to tell people that the internal components of an egg before it’s fertilized are different from an embryo.”
If eggs are damaged in the defrosting process, then they won’t be able to be used in future fertility cycles. Your health care provider should explain to you how they will thaw your eggs or embryos when you decide to use them and what the chances of damage could be. It’s crucial that you feel comfortable that your clinic has experience in both collecting and freezing your eggs or embryos, as well as thawing them.
Freezing eggs vs. embryos: The cost
Before you start any fertility treatment, you’ll likely have a lot of questions for your health care provider. And one of the biggest factors you may need to consider is how much it will all cost. Treatment rates can vary dramatically depending on where you live, and cost can be a barrier for many people.
“In the US, the cost of the drugs alone is $4,000 to $5,000 for one cycle, whether you’re freezing eggs or embryos,” says Dr. Levy.
Egg collection and freezing can cost upward of $10,000 before you add on the cost of medication and any medical tests. You also have to pay to store your eggs. This can cost around $800 per year, depending on the clinic you use. Your medical insurance may cover this, so make sure you reach out and see what support you can receive.
If you have chosen to freeze embryos, then this can be even more expensive. If you’ve elected to use a sperm donor, then the sperm can cost between $300 and $4,000.
"Tell your clinic you care about your success. In your hands, with your embryologist, in your lab, what are your results?”
IVF is available through the NHS in the UK if you meet certain criteria (if you’re under 40 and haven’t got pregnant after two years of unprotected vaginal sex), but fertility preservation is not. So egg or embryo freezing would incur an upfront fee at a private clinic.
The egg collection and freezing process can cost around £3,350. Medication can be another £500 to £1,500, and storage costs can be between £125 and £350 per year.
In Canada, egg freezing can cost between CA$5,000 and CA$10,000 per cycle, and embryo freezing can cost up to CA$15,000. And in Australia, one cycle of egg or embryo freezing will cost you around AU$5,000 to AU$7,000.
If you have any concerns or are confused about how much eggs or embryo freezing will cost, then reach out to your health care provider. Before you start any treatment, they should outline what each part of the process will cost and if there’s any financial support you may be able to access to help you fund your treatment.
Freezing eggs vs. embryos: The takeaway
Family planning can be a really exciting but emotionally charged time. And when faced with the costs and procedures involved with freezing eggs and embryos, it may leave you feeling pretty overwhelmed. That’s totally normal.
“Don’t fixate on global stats,” advises Dr. Levy. “Tell your clinic you care about your success. In your hands, with your embryologist, in your lab, what are your results?” With this data, you can make the best decision about how to move forward for you. That might mean egg freezing, embryo freezing, or deciding to put your plans on ice for a while longer.
Use your health care provider as a support and resource. They should be able to answer any of your questions. And if you’re not sure where to begin, you could ask:


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
“2019 National ART Summary.” Centers for Disease Control and Prevention, 28 Feb. 2022, www.cdc.gov/art/reports/2019/national-ART-summary.html. Accessed 9 Aug. 2022.
“BWH Egg Freezing Counseling Tool (EFCT).” MDCalc, www.mdcalc.com/calc/3937/bwh-egg-freezing-counseling-tool-efct. Accessed 9 Aug. 2022.
Choe, Jennifer, et al. “In Vitro Fertilization.” StatPearls, StatPearls Publishing, 2022. Accessed 9 Aug. 2022.
“Donor Insemination.” American Pregnancy Association, 25 Apr. 2012, americanpregnancy.org/getting-pregnant/donor-insemination/. Accessed 9 Aug. 2022.
“Egg Freezing.” Human Fertilisation and Embryology Authority, www.hfea.gov.uk/treatments/fertility-preservation/egg-freezing/. Accessed 9 Aug. 2022.
“Egg Freezing.” Mayo Clinic, 23 Apr. 2021, www.mayoclinic.org/tests-procedures/egg-freezing/about/pac-20384556. Accessed 9 Aug. 2022.
“Egg Freezing for Future Fertility.” IVF Australia, www.ivf.com.au/egg-freezing-for-future-fertility. Accessed 9 Aug. 2022.
“Embryo Freezing (Cryopreservation).” Cleveland Clinic, my.clevelandclinic.org/health/treatments/15464-embryo-freezing-cryopreservation. Accessed 9 Aug. 2022.
“Fertility Treatment 2019: Trends and Figures.” Human Fertilisation and Embryology Authority, www.hfea.gov.uk/about-us/publications/research-and-data/fertility-treatment-2019-trends-and-figures. Accessed 9 Aug. 2022.
“Freezing Embryos.” Johns Hopkins Medicine, 8 Aug. 2021, www.hopkinsmedicine.org/health/treatment-tests-and-therapies/freezing-embryos. Accessed 9 Aug. 2022.
Ho, Jacqueline R., et al. “A Comparison of Live Birth Rates and Perinatal Outcomes between Cryopreserved Oocytes and Cryopreserved Embryos.” Journal of Assisted Reproduction and Genetics, vol. 34, no. 10, Oct. 2017, pp. 1359–66. Accessed 9 Aug. 2022.
In Vitro Fertilisation (IVF).” Human Fertilisation and Embryology Authority, www.hfea.gov.uk/treatments/explore-all-treatments/in-vitro-fertilisation-ivf/. Accessed 9 Aug. 2022.
“In Vitro Fertilization (IVF).” Mayo Clinic, 10 Sept. 2021, www.mayoclinic.org/tests-procedures/in-vitro-fertilization/about/pac-20384716. Accessed 9 Aug. 2022.
“IVF.” NHS, www.nhs.uk/conditions/ivf/availability/. Accessed 9 Aug. 2022.
“IVF: What Happens.” NHS, www.nhs.uk/conditions/ivf/what-happens/. Accessed 9 Aug. 2022.
“Cost of Egg & Embryo Freezing in the U.S.” Pacific Fertility Center Los Angeles, www.pfcla.com/blog/egg-freezing-costs. Accessed 9 Aug. 2022.
“Age Is the Key Factor for Egg Freezing Success Says New HFEA Report, as Overall Treatment Numbers Remain Low.” Human Fertilisation and Embryology Authority, www.hfea.gov.uk/about-us/news-and-press-releases/2018-news-and-press-releases/press-release-age-is-the-key-factor-for-egg-freezing-success-says-new-hfea-report-as-overall-treatment-numbers-remain-low/. Accessed 9 Aug. 2022.
Son, Weon-Young, and Seang Lin Tan. “Comparison between Slow Freezing and Vitrification for Human Embryos.” Expert Review of Medical Devices, vol. 6, no. 1, Jan. 2009, pp. 1–7. Accessed 9 Aug. 2022.
“Treating Infertility.” The American College of Obstetricians and Gynecologists, www.acog.org/womens-health/faqs/treating-infertility. Accessed 9 Aug. 2022.




