For most people, having a slightly heavier period for a few days is entirely normal. But if you experience a sudden, heavy period or one that lasts longer than expected, you may need to seek medical care.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
When Should You Go to the Hospital for Heavy Menstrual Bleeding?


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
Is every heavy flow considered to be HMB?
Heavy menstrual bleeding (HMB) is also known as menorrhagia. This medical term refers to abnormally heavy or prolonged bleeding. Although it’s quite difficult to estimate the incidence of HMB, it’s somewhere in the range of 5 to 30 percent, according to different sources.
It can be challenging to maintain your normal daily activities with HMB because of significant blood loss. And some bleeding can be very heavy, leading to the need to change your tampon or pad frequently (less than two hours). If you think your periods are like this, talk with your health care provider about possible treatment options.

Irregular cycle?
Discover chatbot and learn more on evaluating symptoms of menopause and other conditions that can cause hair loss.
Various things can cause heavy menstrual bleeding. Here are some of the causes:
- Fibroids and polyps: Uterine fibroids and uterine polyps may cause increased bleeding and irregular periods.
- Adenomyosis: This causes endometrial tissue (lining of the uterus) to grow into the uterine wall. It’s seen in later childbearing years and usually resolves following menopause.
- Endometriosis: This condition causes endometrial-like tissue to grow outside of the uterus. This growth usually occurs on the ovaries and supporting ligaments of the uterus and in the pelvic cavity.
- Irregular ovulation: When ovulation and periods don’t occur regularly, areas of the endometrium (the uterine lining) can become too thick. This irregularity usually happens during puberty, perimenopause, and in people diagnosed with polycystic ovary syndrome and hypothyroidism.
- Bleeding disorders: Some disorders prevent blood from clotting properly, which causes heavy bleeding.
- Medications: Blood thinners can cause heavy menstrual bleeding.
- Intrauterine devices (IUD): IUDs, particularly those containing copper, may also cause heavier menstrual bleeding, especially during the first year following insertion.
- Cancer: Heavy menstrual bleeding can be an early sign of uterine or cervical cancer. Most cases happen in people in their mid-60s who are postmenopausal. With early diagnosis, treatment is highly effective.
- Other causes: Heavy bleeding can be pregnancy-related, in the event of ectopic pregnancy or miscarriage. Pelvic inflammatory disease also can cause heavy menstrual bleeding. Other times, the cause is unknown.

Track symptoms and patterns
Log symptoms to spot patterns in your cycle as they can provide insight into underlying medical conditions
Take a quiz
Find out what you can do with our Health Assistant
What’s normal and what’s not: When to seek medical attention for HMB
Determining if you have heavy menstrual bleeding (as defined medically) can be tricky, because many women may have a different idea of what heavy bleeding actually is. Typically, menstrual bleeding lasts about four to five days, and overall blood loss is minimal (two to three tablespoons). It’s worth noting that menstruation isn’t just blood. It also contains endometrial tissue, so it’s not always easy to estimate actual blood loss.
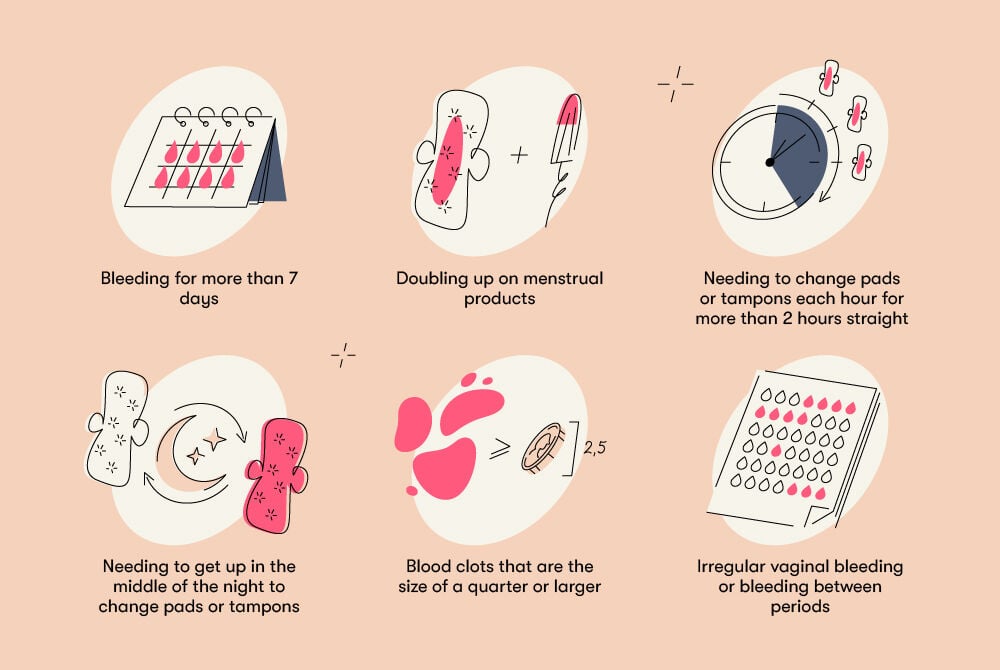
According to the American College of Obstetrics and Gynecology (ACOG), any of the following are signs of heavy menstrual bleeding:
- Bleeding that occurs for more than seven days
- Needing to use a tampon and a pad simultaneously or using more than one pad to prevent leaking
- Vaginal bleeding that’s heavy enough to soak at least one pad or tampon each hour for more than two hours straight
- Needing to get up in the middle of the night to change pads or tampons
- A menstrual flow that includes blood clots that are the size of a quarter or larger
- Irregular vaginal bleeding or bleeding between periods (that isn’t ovulation spotting)
Heavy bleeding can cause anemia, which will make you feel tired and worn out.
If you’re experiencing heavy periods and notice the signs mentioned above, it’s important to tell your health care provider. They may want to see you before your next appointment to evaluate your symptoms further.
Is losing too much blood during your period life-threatening?
You might be asking, when should you go to the hospital for heavy menstrual bleeding? Blood loss from heavy periods can lead to a more severe, urgent medical condition. Heavy blood loss can decrease the amount of circulating blood in the body and the usual amount of oxygen the body needs. So, can losing too much blood during your period be life-threatening? The answer is, if you’re experiencing any of the following while you have heavy vaginal bleeding, you should seek immediate medical attention:
- Shortness of breath
- Chest pain
- Increased heart rate
- Dizziness
- Faintness
How to treat HMB
Treatment options for HMB vary based on the cause, patient age, general health, medical history, medications currently being taken, and the extent of bleeding during each menstrual cycle. Your health care provider may also order tests like blood work or ultrasound to determine the best method of treatment for you. Any plans to have children or not wanting to have a period at all can also affect the treatment used. Ultimately, most people want to reduce the bleeding associated with HMB. It’s absolutely possible to take control of your health and address the issues caused by HMB.
If you’re looking for inspiration, our hero, Lou, shared with us how she successfully managed her HMB and associated conditions and symptoms.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.




