Everything you need to know about toxic shock syndrome, including the causes, symptoms, and how to lower your risk of getting it.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Toxic shock syndrome: Causes, symptoms, and prevention


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
You’ve probably heard of toxic shock syndrome (TSS) before, but what exactly is it, what causes it, and how do you know if you have it? Here, we take an in-depth look at everything you need to know about TSS.
Key takeaways
- TSS is a rare but very serious illness caused by a bacterial infection.
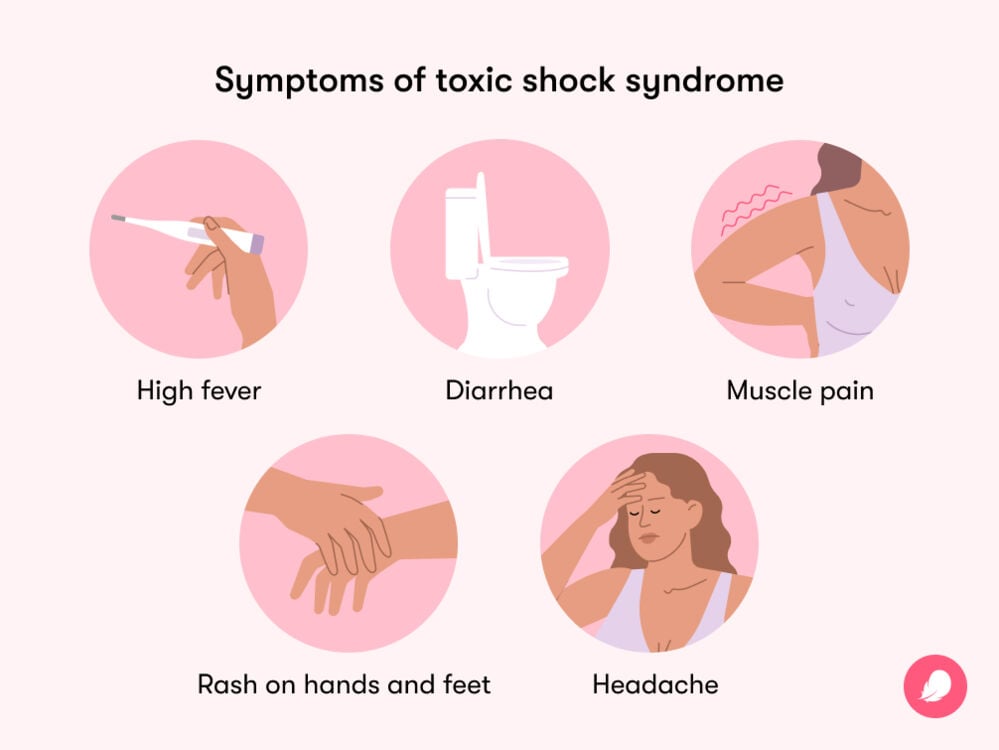
- Signs of TSS can include a high fever, diarrhea, muscle pain, a rash on your hands and feet, and headaches.
- Most people associate TSS with tampons, but anyone can get TSS — including people who don’t have periods.
- Your risk of developing TSS is very low (even if you use tampons).
Toxic shock syndrome (TSS): What is it?
Toxic shock syndrome, or TSS, is a rare but potentially life-threatening illness caused by certain bacterial infections. It happens when bacteria called Staphylococcus aureus (staph) and Streptococcus pyogenes (strep) overgrow and release toxins into the bloodstream.
You might have heard that TSS is caused by using tampons, but it’s a common misconception that TSS is only tampon-related. Nowadays, only half of all cases of TSS have any relation to menstruation.
Most people with periods have probably worried about TSS at some point. Luckily, TSS is rare, and there are things you can do to lower your chances of getting it. Read on to learn more about what causes toxic shock syndrome, toxic shock symptoms, and how to protect yourself.
What causes TSS?
TSS is usually caused by staph bacteria, but it can also be caused by strep bacteria. Staph bacteria typically live on your body; for example, around 30% of people have staph in their noses. The bacteria can then enter your bloodstream through small skin tears or wounds. In comparison, strep can go on to cause TSS in people who have recently had another infection from the bacteria, such as strep throat, and it usually impacts the skin, throat, and anogenital tract.
However, just being exposed to these bacteria doesn’t necessarily mean you’ll develop TSS unless they multiply very quickly and produce a toxin called toxic shock syndrome toxin (TSST).
If this toxin enters your bloodstream, it can cause serious damage to your organs. Although TSS is often thought of as being linked to tampon use, it can also be caused by surgery, skin wounds, menstrual cups, diaphragms, and contraceptive sponges.
It’s important to know that TSS can affect anyone, so it’s crucial to be aware of the symptoms and seek medical attention if necessary.
Can pads cause TSS?
Yes, you can still develop TSS if you wear period pads, although this is considered to be less common than developing TSS from using tampons.
Take a quiz
Find out what you can do with our Health Assistant
How common is it?
As we’ve seen, TSS is rare. It’s thought to affect around one in every 100,000 people, and it’s more common in women. Although your likelihood of getting toxic shock syndrome is very low, it’s still a good idea to know about it and its associated risk factors.
How long does it take to get toxic shock syndrome from a tampon?
There isn’t a defined amount of time that it takes to get TSS from a tampon. That being said, experts recommend removing a tampon after a maximum of eight hours of use because leaving it in longer than this has been linked with TSS. Leaving a tampon in for longer than eight hours doesn’t mean you will definitely get TSS, but it could increase your chances.
Main toxic shock syndrome symptoms
Now that we know what TSS is and what causes it, what are the symptoms to be aware of?
- Symptoms of TSS include:
- A high fever that comes on suddenly
- Diarrhea or vomiting
- Hypotension (low blood pressure)
- Confusion
- A rash that looks like sunburn, especially on the soles of the feet and palms of the hands
- Muscle aches
- Red eyes, throat, and mouth
- Headaches
- Seizures
Toxic shock syndrome symptoms can vary from person to person, depending on the bacteria the infection came from. In most cases, symptoms of TSS start suddenly, just a few hours or days after the bacteria enters your bloodstream.
TSS risk factors
TSS can affect anyone, regardless of gender or whether they use tampons. This includes children, men, and postmenopausal women. While tampons don’t directly cause TSS (rather, it’s the bacteria that can grow on them), it’s important to follow the recommended usage guidelines to reduce risk.
Alongside the risk of leaving in a tampon for more than eight hours, other factors can increase your risk of developing toxic shock, such as:
- Using female barrier contraceptives such as caps, diaphragms, or sponges (types of nonhormonal birth control)
- Having a break in the skin, such as a burn or cut
- Having a viral infection, including chickenpox or flu
- Having recently had surgery
TSS complications
TSS is a life-threatening illness, and, in some cases, it can affect the major organs in your body. If the condition isn’t treated, it can result in complications including:
- Shock
- Renal failure
In extreme scenarios, untreated TSS can even be fatal. This can sound scary, but remember that the condition is very rare, and there are numerous treatment options available (more on those below).
How is TSS diagnosed?
There’s no one test to diagnose toxic shock syndrome. As a first step, your doctor might need to carry out tests to check for staph or strep bacteria. This could involve taking a blood or urine sample or a sample of tissue from your vagina, throat, or cervix and testing them to see if the bacteria is present. Alternatively, your doctor may examine your vagina or take tissue from the site of infection.
Toxic shock syndrome treatment
As TSS can be potentially life-threatening, your treatment will most likely take place in a hospital. If a tampon or contraceptive method is thought to be the cause of TSS, then this will be removed from your vagina right away.
There is no set way to treat TSS following this. However, treatment options can include:
- Antibiotics
- Medication to help stabilize your blood pressure, if needed
- Fluids, if you’re dehydrated
- Surgery, if infected tissue needs to be removed or the infection needs to be drained
Can you prevent TSS?
Here are a few simple tips you can follow to help reduce your risk of developing TSS:
- Change your tampon, pad, or menstrual cup every four to eight hours (or more frequently if your flow is heavy) — setting a reminder on your phone can help.
- Try to alternate using tampons with sanitary pads.
- Always use tampons that have the lowest absorbency you need.
- Only use tampons when you’re on your period, not at other times.
- TSS can reoccur, so if you’ve had it before, avoid using tampons in the future.
- Maintain good hygiene during your period and wash your hands thoroughly before and after you insert a tampon or menstrual cup.
When should I see a doctor?
Always speak to your doctor right away if you’re experiencing any of the symptoms of TSS, particularly if you use tampons, have recently had surgery, or have a cut or wound that appears infected or inflamed. Being quickly examined, diagnosed, and treated will give you the best chance for a positive outcome.
What can you expect from your visit?
As TSS symptoms can come on suddenly, you’re unlikely to have time to prepare in advance for a visit with your doctor. Instead, it’s likely that you will have an urgent or emergency evaluation. With this in mind, it can be helpful to know what to expect from seeing your doctor.
As noted above, due to the serious nature of TSS, you will most likely be seen in a hospital. Your doctor will check for any symptoms of TSS and may ask about any recent injuries or surgeries. As we’ve discussed, they’ll remove any items from your vagina that might be causing TSS. Following this, there are a range of treatment options listed above that might be followed.
FAQs
Is it OK to sleep with a tampon in?
Experts recommend using a pad rather than a tampon at night to lower your risk of getting TSS. After all, if you’re lucky enough to get more than eight hours of sleep, this will take you over the recommended time of leaving a tampon in for a maximum of eight hours.
Is there mild TSS?
If you develop TSS, then your symptoms may be mild to begin with and then get rapidly worse. In some cases, however, your symptoms may remain mild, which is why it’s so important to know what to look out for when considering whether you may have the infection.
What if I accidentally leave a tampon in for more than eight hours?
It happens to the best of us. If you accidentally leave a tampon in for more than eight hours and start noticing any of the signs of TSS, then you should seek medical attention as soon as possible. However, if you’ve left a tampon in for more than eight hours and aren’t experiencing any symptoms, there’s no need to be alarmed.
How quickly does toxic shock syndrome develop?
Toxic shock syndrome develops very quickly. You may initially experience mild symptoms of the infection, but these will rapidly become more severe.
Are toxic shock syndrome symptoms painful?
Yes, TSS symptoms can be painful and uncomfortable. As we’ve seen, these can include a high fever, stomach issues, a rash, headaches, muscle aches, and more.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
Suen, Jeffrey, et al. “Chapter 71: Toxic Shock Syndrome.” Feigin and Cherry’s Textbook of Pediatric Infectious Diseases (Sixth Edition), edited by Ralph D. Feigin et al. W.B. Saunders, 2009, pp. 862–84,
doi.org/10.1016/B978-1-4160-4044-6.50076-5.
“Group A Streptococcal Infections.” Public Health Scotland, 30 Aug. 2023, www.hps.scot.nhs.uk/a-to-z-of-topics/streptococcal-infections/group-a-streptococcal-infections/.
Sharma, Hema, et al. “Toxic Shock Syndrome Toxin 1 Evaluation and Antibiotic Impact in a Transgenic Model of Staphylococcal Soft Tissue Infection.” mSphere, vol. 4, no. 5, 9 Oct. 2019, doi.org/10.1128/mSphere.00665-19.
“Staphylococcus Aureus in Healthcare Settings.” Centers for Disease Control and Prevention, www.cdc.gov/hai/organisms/staph.html. Accessed 20 Sep. 2023.
“Toxic Shock Syndrome.” Cleveland Clinic, my.clevelandclinic.org/health/diseases/15437-toxic-shock-syndrome. Accessed 20 Sep. 2023.
“Toxic Shock Syndrome (TSS).” Johns Hopkins Medicine, www.hopkinsmedicine.org/health/conditions-and-diseases/toxic-shock-syndrome-tss. Accessed 20 Sep. 2023.
“Toxic Shock Syndrome.” Mayo Clinic, 23 Mar. 2022, www.mayoclinic.org/diseases-conditions/toxic-shock-syndrome/symptoms-causes/syc-20355384.
“Toxic Shock Syndrome.” NHS, www.nhs.uk/conditions/toxic-shock-syndrome/. Accessed 20 Sep. 2023.
“Your First Period.” The American College of Obstetricians and Gynecologists, June 2022, www.acog.org/womens-health/faqs/your-first-period.




