Know what normal vaginal discharge looks like and how it changes throughout your cycle — plus, find out how to spot abnormal discharge.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Normal vs. abnormal vaginal discharge: What’s the difference?


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
A lot of us have been made to feel as though discharge is “gross” or a problem. When actually, it’s the opposite! Typical discharge is a sign that your body is keeping you clean and healthy and working to protect you against infections. And abnormal discharge — whether it’s a change in color, consistency, or smell — is your body communicating that something’s up.
Both functions are pretty clever if you ask us. But with so much discharge variation throughout your cycle and over your lifetime, the big question is: How do you know what’s normal and what’s not?
Enter Flo, with a little help from Dr. Sara Twogood, obstetrician and gynecologist, Cedars-Sinai Medical Group, California, US.
Key takeaways
- Normal discharge is usually clear or whitish, mild-odored, and can range from feeling wet and slippery to sticky and gooey or thick and creamy to drier and more pasty.
- However, discharge varies depending on the person, where they are in their cycle, and other factors. So the key is to understand your baseline; then, it’ll be easier to know when something’s off.
- Factors that might impact what “normal” discharge looks like for you include pregnancy, menopause, birth control, and other medications.
- Abnormal discharge can include discharge that is yellow, green, frothy, clumpy, and fishy- or foul-smelling. These are potential signs of infection, so if you notice them, give a health care professional a call.
What does normal discharge look like?
While it can slightly differ for everyone, “normal” or healthy discharge is typically clear, white, or off-white and can feel wet and slippery, sticky and gooey, thick and creamy, or drier and more pasty. It’s typical to notice around .5 to 1 tsp or 2.5 to 5 ml of it in your underwear every day.
“But ultimately, ‘normal’ discharge really varies,” says Dr. Twogood, “and lots of different factors will determine what it looks like for any one person.”
Take a quiz
Find out what you can do with our Health Assistant
Discharge changes as your hormones shift throughout the menstrual cycle. Your cycle can be split into two phases — the follicular phase and the luteal phase. In between these two phases is ovulation — the point in your cycle where one of your ovaries releases an egg to be potentially fertilized by a sperm.
Ovulation, your period, and the different phases of your cycle are all driven by the rise and fall of your sex hormones like estrogen and progesterone. Estrogen plays an important role in supporting you as you have your period and potentially prepare for pregnancy and can impact the way your discharge looks and feels.
Dr. Twogood points out, “That’s why it’s important to understand your baseline and then keep an eye out for red flags or changes to that baseline that feel unusual for you.” (More on these red flags in a sec.)
Some textbook discharge types you might notice throughout your cycle include:
- A creamy white discharge earlier in your menstrual cycle, after your period
- Egg white discharge, aka clear and slippery discharge resembling raw egg whites right before ovulation
- A white, dry, or sticky discharge after ovulation
If you want to keep an eye on changes in your vaginal discharge and better understand your body’s “baseline” and patterns, it can help to log them in a period-tracking app like Flo.
What does abnormal vaginal discharge look like?
Now, let’s dive a little deeper into those discharge “red flags” Dr. Twogood mentioned — and what they could mean.
- Clumpy white discharge: White discharge can be perfectly normal. But if it’s clumpy like cottage cheese and accompanied by itching and irritation around your vulva, it could point to a yeast infection.
- Yellow/green discharge: Light yellow discharge can be normal, but if it’s also a clumpy consistency (like cottage cheese), it could be a yeast infection. If you have a darker yellow, yellow-green, or straight-up green discharge, it could be a sign that you have an infection, especially if there’s also a change in the consistency and smell of the discharge.
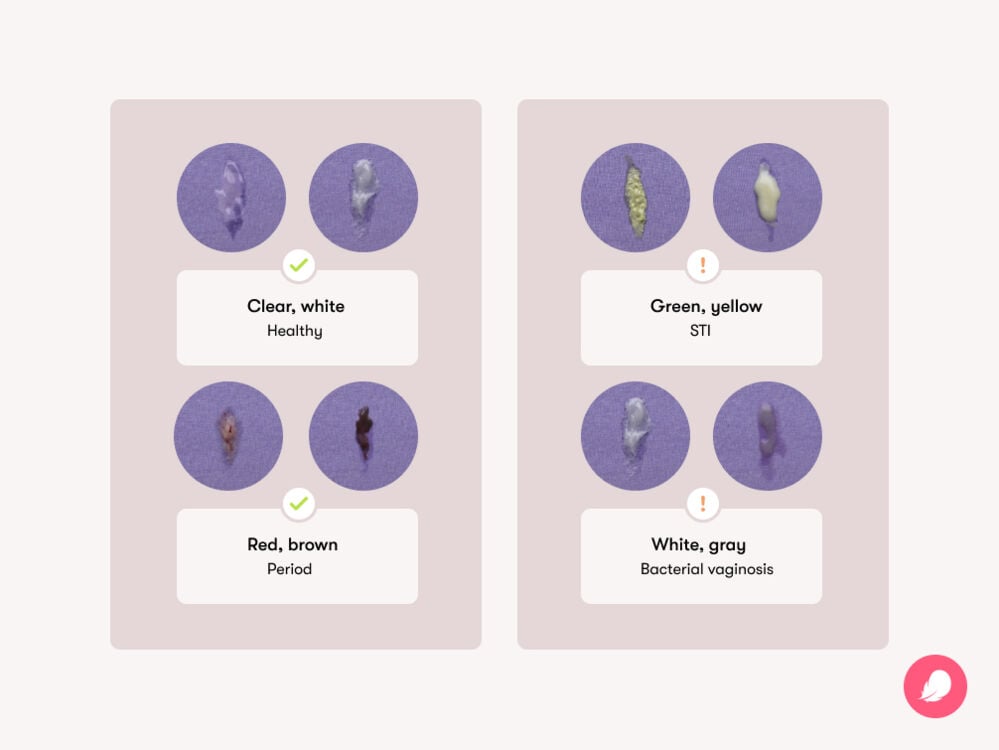
- Gray discharge: Gray discharge that is thin and watery and has a strong fishy smell could be signaling an infection called bacterial vaginosis (BV).
- Pink/brown discharge: Pink discharge and brown discharge can show up when a bit of blood mixes with your discharge. If it happens around your period or implantation (when some folks get spotting), it can be normal. But if it’s accompanied by any uncomfortable symptoms, like pain, itching, or irritation, it could be an infection.
Generally, Dr. Twogood summarizes, “If you’re noticing any types of discharge that feel unusual for you, whether it’s the color, texture, or amount, or you have any other symptoms that are worrisome — like irritation, inflammation, or pain when urinating — then make an appointment with a health care professional.”
How does normal vs. abnormal vaginal discharge smell?
The first thing to know is that normal vaginal discharge does have a smell.
“We’re often made to feel like our discharge, and our vulvas in general, shouldn’t smell of anything,” Dr. Twogood says. “‘Feminine hygiene products are marketed to us to cover up smells.” But certain smells are healthy.
The smell of healthy vaginal discharge might change, she explains, depending on the time of your cycle, what you’ve been eating, and more. “But it tends to have a slightly tangy or acidic smell to it. It might smell more metallic around your period. And the bottom line is it shouldn’t smell noticeably bad.”
Foul-smelling discharge could be hinting at an infection. And as we covered, a specifically fishy odor is a sign of bacterial vaginosis or trichomoniasis, particularly when coupled with unusual discharge colors or textures. So, if you’re noticing any of that, raise it with a healthcare professional.
What else can affect the type of discharge you have?
The short answer here is a whole lot of things. So it’s hard to be exhaustive. But, besides cycle phase and infections, some common factors that can cause changes to your discharge include:
- Hormonal birth control: With the pill and other hormonal birth control, you might notice heavier or more frequent discharge. If you’re experiencing spotting or breakthrough bleeding from your contraception, your discharge may also, at times, be tinged with a pink or brown color.
- Perimenopause and menopause: Lower estrogen levels in the lead-up to menopause (called perimenopause) can mean your body produces less discharge. During this time, your discharge could also be tinged with blood (i.e., appear brownish) because the lining of your vagina gets drier and thinner, which can cause light bleeding or spotting. If you notice blood in your discharge or it appears pink or brown, then reach out to a health care professional. They’ll be able to get to the bottom of what could be causing it and ease your discomfort.
- Pregnancy: It’s common to notice increased discharge in pregnancy, and it might be extra mucus-like. Your body produces extra cervical mucus in pregnancy to help protect the baby by preventing bacteria from going up the vagina and cervix.
- Douches or cleansers: Vaginal douches can upset the natural pH levels in your vagina, which can make you vulnerable to infection and cause abnormal discharge. The same is true of scented soaps and cleansing products. (All you need is warm water to clean your vulva.)
How to maintain normal, healthy discharge
Luckily, it’s really easy to maintain healthy discharge. You can:
- Wash your vulva regularly with warm water (if you want to use soap, ensure it’s mild and unscented — and remember, no perfumed products and no douching).
- Wear breathable cotton underwear (Dr. Twogood adds that sleeping with no underwear can be beneficial, too).
- Stay protected during sex (condoms will reduce your risk of STIs and other infections that disrupt your vagina’s pH levels, like BV).
More frequently asked questions about normal vs. abnormal vaginal discharge
Is it normal to have vaginal discharge every day?
Yes! It’s normal to notice around .5 to 1 tsp or 2.5 to 5 ml of discharge in your underwear every day. If you’re pregnant, ovulating, or on birth control, you might notice more discharge than usual. If you’re menopausal, you might notice less.
How to check vaginal discharge
You can look at it in your underwear or on the toilet paper when you wipe. Or, if you want to check it with your hands, insert a clean finger into your vulva and then, between your thumb and index finger, rub the discharge around or separate your fingers to observe the consistency.
What does BV discharge look like?
Some people with BV will notice an abnormal discharge that is white or gray, thin or watery and smells strongly of fish. This may be more noticeable during and after sex and when you’re on your period.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
“Bacterial Vaginosis.” Cleveland Clinic, my.clevelandclinic.org/health/diseases/3963-bacterial-vaginosis. Accessed 11 Oct. 2024.
“Brown Discharge: 4 Causes and What It Means.” Cleveland Clinic, 25 July 2022, health.clevelandclinic.org/brown-vaginal-discharge.
“Cervical Mucus.” Cleveland Clinic, my.clevelandclinic.org/health/body/21957-cervical-mucus. Accessed 11 Oct. 2024.
“Is Breakthrough Bleeding More Common with Extended-Cycle Birth Control Pills, Such as Seasonale and Others?” Mayo Clinic, 7 Dec. 2022, www.mayoclinic.org/healthy-lifestyle/birth-control/expert-answers/seasonale-side-effects/faq-20058109.
“Follicular Phase.” Cleveland Clinic, my.clevelandclinic.org/health/body/23953-follicular-phase. Accessed 11 Oct. 2024.
Lacroix, Guillaume, et al. “The Cervicovaginal Mucus Barrier.” International Journal of Molecular Sciences, vol. 21, no. 21, 4 Nov. 2020, p. 8266, doi:10.3390/ijms21218266.
“Mucus Plug.” Cleveland Clinic, my.clevelandclinic.org/health/symptoms/21606-mucus-plug. Accessed 11 Oct. 2024.
Sobel, Jack D. “Patient Education: Vaginal Discharge in Adult Women (Beyond the Basics).” UpToDate, 13 Mar. 2023, www.uptodate.com/contents/vaginal-discharge-in-adult-women-beyond-the-basics/print.
Thiyagarajan, Dhanalakshmi K., et al. “Physiology, Menstrual Cycle.” StatPearls, StatPearls Publishing, 2024, www.ncbi.nlm.nih.gov/books/NBK500020/.
“Thrush in Men and Women.” NHS, www.nhs.uk/conditions/thrush-in-men-and-women/. Accessed 11 Oct. 2024.
“Vaginal Discharge.” NHS Inform, 1 June 2023, www.nhsinform.scot/illnesses-and-conditions/sexual-and-reproductive/vaginal-discharge/.
“Vaginal Discharge.” NHS, www.nhs.uk/conditions/vaginal-discharge/. Accessed 11 Oct. 2024.
“Vaginal Discharge.” Cleveland Clinic, my.clevelandclinic.org/health/symptoms/4719-vaginal-discharge. Accessed 11 Oct. 2024.
“Vaginal Discharge Color: What’s Normal and What Isn’t.” Cleveland Clinic, 29 July 2022, health.clevelandclinic.org/vaginal-discharge-mean.
“Vaginal Dryness.” MedlinePlus, medlineplus.gov/ency/article/000892.htm. Accessed 11 Oct. 2024.
“Vaginal Odor.” Cleveland Clinic, my.clevelandclinic.org/health/symptoms/17905-vaginal-odor. Accessed 11 Oct. 2024.
“What Ovulation Signs Can I Watch for if I Want to Get Pregnant?” Mayo Clinic, 9 July 2024, www.mayoclinic.org/healthy-lifestyle/getting-pregnant/expert-answers/ovulation-signs/faq-20058000.
“Yeast Infection (Vaginal).” Mayo Clinic, 11 Jan. 2023, www.mayoclinic.org/diseases-conditions/yeast-infection/symptoms-causes/syc-20378999.




