From an increased sex drive to insomnia, here’s the lowdown on being 14 weeks pregnant.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
14 weeks pregnant: Your guide to this week of your second trimester

Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
Welcome to your second trimester! At 14 weeks pregnant, you’ve made it through the period when you were most likely not to feel well because of pregnancy symptoms, with 70% of pregnant women experiencing nausea in the first trimester. Hopefully, you are starting to feel better now or can look forward to feeling more comfortable in the coming weeks.
You’re probably full of questions about what this trimester will bring, as well as specifically what to expect now that you’re 14 weeks pregnant. Keep reading to discover how your baby is developing, the most common pregnancy symptoms at this stage, and lifestyle tips for a healthy baby and mom, with advice from a Flo expert.
Your baby at 14 weeks pregnant
Forming toenails
Now that you’re 14 weeks pregnant, your baby is starting to form tiny toenails, which will be fully developed by 36 weeks. Adorable.
Forming fetal red blood cells
At this stage, your baby is also forming fetal red blood cells, which are currently produced in your baby’s spleen. By the third trimester, their bone marrow will take over. This is where these important cells, which carry oxygen around the body, will be created for the rest of your baby’s life.
How big is a baby at 14 weeks pregnant?
Length (crown to heel): 14.7 cm or 5.8 in.
Weight: 93 g or 3.3 oz.
Size: Equivalent to a peach
All measurements are approximate and vary within the normal range.
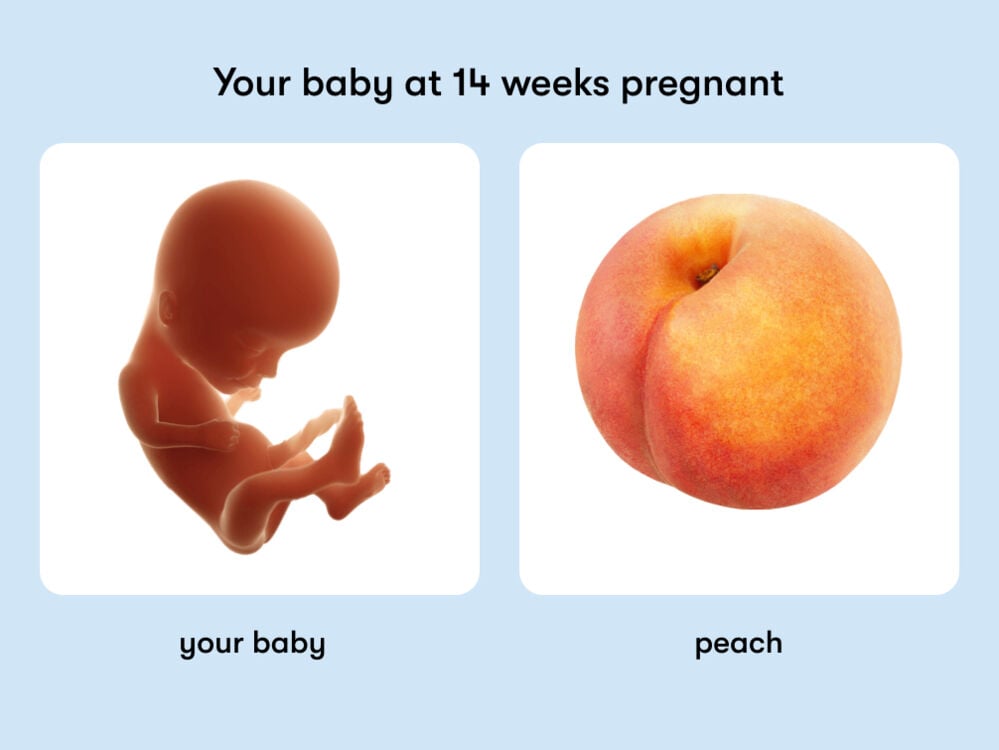
Your body at 14 weeks pregnant
Increased sex drive and heightened sensitivity during sex
Found yourself feeling a bit friskier lately? It might come as a surprise, but around now, changes to your pregnancy hormones can result in an increased sex drive. A 2020 study found that desire increased in the second trimester for some women, after initially dipping in the first.
And another bonus? Increased blood flow to the vulva at this stage can also heighten sensitivity during sex — a second-trimester pregnancy symptom we can definitely celebrate.
While these changes are common in the second trimester, it’s also natural not to get them. After all, every pregnancy is different, so try not to compare yourself to others. And if you haven’t experienced them yet, then you never know, they might be coming your way very soon!
Insomnia
At the start of your second trimester, you may have noticed a pregnancy symptom that’s definitely not as fun: insomnia. And as your pregnancy develops, the physical changes to your body, such as your growing bump and other pregnancy symptoms, can continue to disturb your sleep.
“Insomnia is common throughout pregnancy,” explains Dr. Jenna Beckham, obstetrician and gynecologist, WakeMed, North Carolina, US. “It can increase during the course of pregnancy and may affect two-thirds of pregnant people by the end of the third trimester. There are many factors that can lead to insomnia, including but not limited to nausea, urinary frequency, backache/pain, fetal movement, heartburn, leg cramps, and physical limitations to finding a comfortable position for sleeping.”
Insomnia can be very frustrating to deal with, but luckily, there are a few things you can try to make yourself more comfortable throughout the night. For example, your doctor may recommend that you start sleeping on your side or putting a pillow between your knees and under your bump for added support. Dr. Beckham also has some advice to share. “Unless treatment is needed for a specific condition, like reflux, most interventions to improve sleep are behavioral,” she explains. “Examples include maintaining a regular sleep schedule, limiting liquid intake before bedtime, and avoiding afternoon caffeine intake. If pharmacotherapy is needed, melatonin should be tried first. If this is not effective, antihistamines such as doxylamine and diphenhydramine can be used.” Remember, you should always speak to your doctor before taking any new medications.
Take a quiz
Find out what you can do with our Health Assistant
Your questions answered
Can you feel a baby at 14 weeks?
While your baby might be moving around when you’re 14 weeks pregnant, it’s unlikely that you’ll be able to feel them just yet.
If this is the case, then don’t worry. “Some patients may start to feel some movement by 14 weeks, but it is perfectly normal if movement is not yet felt,” explains Dr. Beckham. Generally, you'll feel first movements between 16-24 weeks.
What should you feel at 14 weeks pregnant?
Many women find that they feel the best physically in their second trimester. Not only should any nausea (finally) start to calm down, but fatigue and breast tenderness can also begin to subside.
However, for some women, the loss of these pregnancy symptoms can bring new bouts of anxiety. It’s natural to worry if you stop experiencing your usual pregnancy symptoms. However, if you’re starting to feel more like your normal self, know that this doesn’t necessarily mean that there is anything wrong with you or your baby. Remember that you can always reach out to your doctor if you have any questions or concerns and seek support from your loved ones if you’re finding it tough to adjust to the (many) changes happening in your body.
Plus, at 14 weeks pregnant, it’s still very early in your second trimester, so you may actually still be experiencing some symptoms of pregnancy from the earlier weeks, from nausea to mood swings. If you are, hang in there and know that these symptoms are likely to pass soon.
Should I be showing at 14 weeks?
Some women find that they start showing at 14 weeks, whereas others might not notice a bump until 16 weeks. Everybody is different, so don’t panic if you haven’t noticed any major changes to your tummy just yet. At around 12 weeks pregnant, some women start to notice a small bump. But if it’s not your first pregnancy, you may have noticed a bump growing sooner, which is likely due to the fact that your stomach muscles have been stretched before.
“The appearance of a ‘bump’ varies greatly depending on each individual’s body shape and size,” says Dr. Beckham. So try not to compare yourself to others too much. Your bump will develop in its own beautiful way.
Your 14 weeks pregnant checklist
Eat iron-rich food
From the second trimester, your body starts requiring more iron. This is because the amount of blood in your body increases by a massive 50% to 60% during pregnancy, and you need iron to develop healthy red blood cells to deliver oxygen to your baby.
Certain foods are a great source of iron, so make sure you’re eating plenty of the following:
- Pulses and beans
- Nuts and seeds
- Dried fruits (e.g., dried apricots, prunes, and raisins)
- Dark-green leafy vegetables (e.g., watercress and kale)
- Iron-fortified cereal or bread
- Brown rice
- Eggs (these must be well cooked)
- White and red meat
- Fish
- Tofu
To make sure you’re getting all the extra iron you need during pregnancy, it can also be a good idea to take a prenatal vitamin that contains iron. However, you should always have a chat with your doctor first before starting any new vitamins or supplements.
Consider prenatal exercise
At 14 weeks pregnant, now can be a great time to try prenatal exercise. For example, yoga or Pilates modified for pregnancy are safe ways to reduce stress, improve flexibility, and encourage focused breathing. Brisk walking is another safe way to exercise during pregnancy, offering a total-body workout that won’t put extra strain on your joints or muscles.
In general, it’s good to aim for at least 150 minutes of moderate-intensity exercise (when you’re moving enough to increase your heart rate and sweat) each week while you’re pregnant. It’s always worth checking in with your doctor before you start any new exercise routine though, just in case.
You may also want to consider a prenatal class. While most classes start when you’re around 30 to 32 weeks pregnant, they often get booked up quickly. If you start looking now, you might be more likely to get a spot in your first choice of class.
Your prenatal class will teach you how to stay healthy during pregnancy, how to care for and feed your baby, as well as how to make a birth plan and choose from the different options you have for labor. Not only that, but it’s a brilliant opportunity to make new friends with people having babies around the same time as you. These people may end up being a lifeline of emotional support during the initial months of life with your baby.
Invest in a good moisturizer
Itchy, dry skin is common during pregnancy and can often be relieved by applying lotion or moisturizer. There are plenty of pregnancy-safe moisturizers available, so why not treat yourself? Other things that can soothe itchy skin include taking a cool bath, wearing loose clothing made from natural materials (like cotton), and avoiding products that contain strong perfumes.
Itchiness can also be the first sign of stretch marks as the skin starts to become thinner. Stretch marks are very common during pregnancy, with up to 90% of women getting them. Pregnancy stretch marks are caused by the middle layer of skin becoming stretched and broken as your body changes, as well as by hormonal changes that impact your skin. They tend to appear on your tummy as narrow lines that are pink, red, purple, or brown, depending on your skin tone. You might also find stretch marks on your thighs or breasts as they get bigger.
Stretch marks tend to appear as your pregnancy progresses and your bump starts to grow. However, although your bump may start to show anytime from around 12 weeks, stretch marks tend to be caused by growth later on in pregnancy, during the third trimester.
Stretch marks should fade a few months after you’ve given birth, but they probably won’t disappear completely. Be wary of any products that promise to make your stretch marks disappear, as there is no proof that these will actually work.
It can be hard adjusting to the physical changes happening to your body, from pregnancy weight gain to varicose veins. But stretch marks — and any other pregnancy symptoms, for that matter — are definitely nothing to be ashamed of.
When to consult a doctor at 14 weeks pregnant
In the second trimester, you may have prenatal appointments around every four weeks, but it depends on where you live and your pregnancy needs. At these checkups, the doctor will take your blood pressure and ask you to do a urine test. These tests help your doctor check for a range of health concerns, including high sugar levels, infections, and whether you’re at risk of developing preeclampsia, a pregnancy complication causing high blood pressure. They’ll also check your weight and your baby’s heart activity. From 20 weeks pregnant, they’ll also measure the distance from your public bone to your uterus (the fundal height) to see how your baby is growing — all good stuff to help you know that everything is progressing well.
You don’t need to wait until your appointment if you have any concerns or questions about your pregnancy. However, at 14 weeks pregnant, you should contact your doctor immediately if you experience:
- Severe cramping
- Vaginal bleeding
- Changes in vaginal discharge
- Fever
- Dizziness or fainting
- Severe vomiting
This isn’t an exhaustive list and just an example of some of the changes you should look out for. Some of these can be a sign of miscarriage or other health complications, so it’s essential that you speak to your doctor about the best next step for you. And if you’re ever worried about any other symptoms you experience during pregnancy, then don’t hesitate to reach out to your health care provider.
14 weeks pregnant: The takeaway
You’re at the start of your second trimester and beginning a new chapter in your pregnancy. While some women may feel the baby moving or notice a small bump at this stage, it’s more likely that these signs will come later. So don’t worry if you don’t feel that different yet and know that you’ve got it all to look forward to.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
“Anaemia in Pregnancy.” Hull University Teaching Hospitals NHS Trust, 28 Feb. 2019, www.hey.nhs.uk/patient-leaflet/anaemia-in-pregnancy-2/.
“Antenatal Classes.” NHS, www.nhs.uk/pregnancy/labour-and-birth/preparing-for-the-birth/antenatal-classes/. Accessed 1 June 2023.
“Bleeding during Pregnancy.” The American College of Obstetricians and Gynecologists, May 2021, www.acog.org/womens-health/faqs/bleeding-during-pregnancy.
“Bleeding during Pregnancy.” Mayo Clinic, 20 Jan. 2022, www.mayoclinic.org/symptoms/bleeding-during-pregnancy/basics/when-to-see-doctor/sym-20050636.
Brennan, Miriam, et al. “The Use of Anti Stretch Marks’ Products by Women in Pregnancy: A Descriptive, Cross-Sectional Survey.” BMC Pregnancy and Childbirth, vol. 16, no. 1, Sep. 2016, bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/s12884-016-1075-9.
“Exercise during Pregnancy.” The American College of Obstetricians and Gynecologists, Mar. 2022, www.acog.org/womens-health/faqs/exercise-during-pregnancy.
Fernández-Carrasco, Francisco Javier, et al. “Changes in Sexual Desire in Women and Their Partners during Pregnancy.” Journal of Clinical Medicine Research, vol. 9, no. 2, Feb. 2020, https://doi.org/10.3390/jcm9020526.
“Fetal Development: What Happens during the 2nd Trimester?” Mayo Clinic, 3 June 2022, www.mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/in-depth/fetal-development/art-20046151.
Curran, Mark A. “Fetal Development.” Perinatology.com, perinatology.com/Reference/Fetal%20development.htm. Accessed 15 June 2023.
Friel, Lara A. “Fevers during Pregnancy.” MSD Manual Consumer Version, Oct. 2021, www.msdmanuals.com/home/women-s-health-issues/pregnancy-complicated-by-disease/fevers-during-pregnancy.
“Fundal Height.” Cleveland Clinic, my.clevelandclinic.org/health/diagnostics/22294-fundal-height. Accessed 15 June 2023.
“Sex during Pregnancy: Your Questions Answered.” Cleveland Clinic, 30 Apr. 2020, health.clevelandclinic.org/sex-during-pregnancy-your-questions-answered/.
“How Does a Second Pregnancy Differ from the First?” Tommy’s, www.tommys.org/pregnancy-information/im-pregnant/ask-a-midwife/how-does-second-pregnancy-differ-first. Accessed 1 June 2023.
“How Your Baby Develops Week to Week.” NHS Inform, 25 Jan. 2023, www.nhsinform.scot/ready-steady-baby/pregnancy/your-baby-s-development/how-your-baby-develops-week-to-week.
Institute of Medicine (US) Committee on Nutritional Status during Pregnancy and Lactation. “Iron Nutrition during Pregnancy.” Nutrition during Pregnancy. National Academies Press, 1990, www.ncbi.nlm.nih.gov/books/NBK235217/.
Hill, Mark. A. “Integumentary System: Nail Development.” Embryology, embryology.med.unsw.edu.au/embryology/index.php/Integumentary_System_-_Nail_Development. Accessed 1 June 2023.
“Iron Deficiency Anemia during Pregnancy: Prevention Tips.” Mayo Clinic, 9 Feb. 2022, www.mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/in-depth/anemia-during-pregnancy/art-20114455.
“Morning Sickness.” Cleveland Clinic, my.clevelandclinic.org/health/diseases/16566-morning-sickness-nausea-and-vomiting-of-pregnancy. Accessed 1 June 2023.
“Morning Sickness: Nausea and Vomiting of Pregnancy.” The American College of Obstetricians and Gynecologists, May 2020, www.acog.org/womens-health/faqs/morning-sickness-nausea-and-vomiting-of-pregnancy.
“Nutrition during Pregnancy.” The American College of Obstetricians and Gynecologists, May 2023,
www.acog.org/womens-health/faqs/nutrition-during-pregnancy.
Pacheco, Danielle. “Sleeping While Pregnant: Second Trimester.” Sleep Foundation, 15 June 2009, www.sleepfoundation.org/pregnancy/sleeping-during-2nd-trimester.
“Prenatal Care: 2nd Trimester Visits.” Mayo Clinic, 4 Aug. 2022, www.mayoclinic.org/healthy-lifestyle/pregnancy-week-by-week/in-depth/prenatal-care/art-20044581.
“Quickening In Pregnancy: First Movements & What to Expect.” Cleveland Clinic, my.clevelandclinic.org/health/symptoms/22829-quickening-in-pregnancy. Accessed 1 June 2023.
“Red Blood Cells: Function & Role.” Cleveland Clinic, my.clevelandclinic.org/health/body/21691-function-of-red-blood-cells. Accessed 1 June 2023.
Reichner, Cristina A. “Insomnia and Sleep Deficiency in Pregnancy.” Obstetric Medicine, vol. 8, no. 4, Dec. 2015, pp. 168–71, https://doi.org/10.1177/1753495X15600572.
“Second Trimester Worries.” Tommy’s, www.tommys.org/pregnancy-information/im-pregnant/pregnancy-calendar/second-trimester-worries. Accessed 1 June 2023.
Singh, Ranbir, et al. “Embryology, Hematopoiesis.” StatPearls, StatPearls Publishing, 8 Aug. 2022, www.ncbi.nlm.nih.gov/books/NBK544245/.
“Skin Conditions during Pregnancy.” The American College of Obstetricians and Gynecologists, July 2022, www.acog.org/womens-health/faqs/skin-conditions-during-pregnancy.
Soma-Pillay, Priya, et al. “Physiological Changes in Pregnancy.” Cardiovascular Journal of Africa, vol. 27, no. 2, Mar.–Apr. 2016, pp. 89–94, www.ncbi.nlm.nih.gov/pmc/articles/PMC4928162/.
“Stretch Marks.” Mayo Clinic, 12 Jan. 2023, www.mayoclinic.org/diseases-conditions/stretch-marks/symptoms-causes/syc-20351139.
“Stretch Marks in Pregnancy.” NHS, www.nhs.uk/pregnancy/related-conditions/common-symptoms/stretch-marks/. Accessed 15 June 2023.
“The Second Trimester.” Johns Hopkins Medicine, 8 Aug. 2021, www.hopkinsmedicine.org/health/wellness-and-prevention/the-second-trimester.
“Tiredness and Sleep Problems.” NHS, www.nhs.uk/pregnancy/related-conditions/common-symptoms/tiredness/. Accessed 1 June 2023.
“Urgent Maternal Warning Signs.” Centers for Disease Control and Prevention, 27 Feb. 2023, www.cdc.gov/hearher/maternal-warning-signs/index.html.
“Vaginal Discharge in Pregnancy.” NHS, www.nhs.uk/pregnancy/related-conditions/common-symptoms/vaginal-discharge/. Accessed 14 June 2023.
Vine, Tya, et al. “Melatonin Use during Pregnancy and Lactation: A Scoping Review of Human Studies.” Revista Brasileira de Psiquiatria, vol. 44, no. 3, May–June 2022, pp. 342–48, https://doi.org/10.1590/1516-4446-2021-2156.
“Vomiting and Morning Sickness.” NHS, www.nhs.uk/pregnancy/related-conditions/common-symptoms/vomiting-and-morning-sickness/. Accessed 1 June 2023.
“Week 14.” NHS, www.nhs.uk/start4life/pregnancy/week-by-week/2nd-trimester/week-14/. Accessed 1 June 2023.
“What Is Pre-Eclampsia and What Are the Warning Signs?” NHS, www.nhs.uk/conditions/pre-eclampsia/. Accessed 15 June 2023.
“Your Antenatal Appointment Schedule.” Tommy’s, www.tommys.org/pregnancy-information/im-pregnant/antenatal-care/your-antenatal-appointment-schedule. Accessed 15 June 2023.
History of updates
Current version (05 July 2023)
Published (24 February 2019)
In this article
Get your personal guide to pregnancy with the Flo app
-
Follow your baby's growth week by week
-
Get expert info on symptoms, safe foods, and more
-
Chat with other parents-to-be




