Cervical mucus isn’t talked about much, but it plays an important role in your cycle tracking, especially if you’re trying to conceive. Here’s what you need to know.
-
Tracking cycle
-
Getting pregnant
-
Pregnancy
-
Help Center
-
Flo for Partners
-
Anonymous Mode
-
Flo app reviews
-
Flo Premium New
-
Secret Chats New
-
Symptom Checker New
-
Your cycle
-
Health 360°
-
Getting pregnant
-
Pregnancy
-
Being a mom
-
LGBTQ+
-
Quizzes
-
Ovulation calculator
-
hCG calculator
-
Pregnancy test calculator
-
Menstrual cycle calculator
-
Period calculator
-
Implantation calculator
-
Pregnancy weeks to months calculator
-
Pregnancy due date calculator
-
IVF and FET due date calculator
-
Due date calculator by ultrasound
-
Medical Affairs
-
Science & Research
-
Pass It On Project New
-
Privacy Portal
-
Press Center
-
Flo Accuracy
-
Careers
-
Contact Us
Cervical mucus: Everything you need to know about your ovulation discharge


Every piece of content at Flo Health adheres to the highest editorial standards for language, style, and medical accuracy. To learn what we do to deliver the best health and lifestyle insights to you, check out our content review principles.
Most women and people who menstruate have vaginal discharge, but did you know that cervical mucus, also known as cervical fluid or occasionally ovulation discharge, is integral to your cycle?
Initially, it might not seem that important to get into the nitty-gritty of discharge, but if you’re trying for a baby, it’s important to understand cervical mucus because it can often reveal when you’re ovulating and therefore at your most fertile.
Even if you’re not currently trying to conceive, getting to know what’s happening inside your body can be very empowering.
Every one of us is different when it comes to the type, amount, and texture of discharge and cervical fluid we produce, so knowing what’s healthy for you and your cycle can be reassuring. You’ll also be more prepared to look for changes in your discharge (maybe color or smell) that could signal that something’s not quite right.
That said, cervical mucus isn’t necessarily something you learn about at school, so you can be forgiven for not knowing much about it. We spoke with Dr. Jennifer Boyle, obstetrician and gynecologist at Massachusetts General Hospital, Massachusetts, US, to help fill in the blanks.
What is cervical mucus? Is it the same as discharge?
First up, a bit of a biology lesson. Vaginal discharge is a catchall term for everything your vagina produces throughout your cycle. And it has a pretty important function: to keep your vagina healthy by removing dead cells and bacteria. You might notice that the amount, texture, and color (typically clear to milky white) of your discharge changes throughout the month. This is completely normal.
Think of cervical mucus as just one ingredient that makes up your discharge. As its name suggests, this fluid comes from the glands in and around the cervix, rather than the vagina itself — but it has an equally important role to play.
The cervix is a small but mighty, doughnut-shaped part of your reproductive system, “made up of two types of cells,” explains Dr. Boyle. Usually around an inch (2.5 cm) long, it joins the top of your vagina to the lower part of your uterus. “The outside part of the cervix is covered by ‘squamous cells’ that are like skin and the vagina. The inside part of the cervix is made up of ‘glandular cells,’ and these produce cervical mucus,” says Dr. Boyle. “This is different than the secretions, or discharge, of the vagina.”
So what’s the mucus for? “The main role of cervical mucus is to help transport sperm into the uterus and then up to the tubes around the time of ovulation. It then provides a protective barrier after ovulation to keep things from getting inside the uterus,” explains Dr. Boyle. “The appearance and amount of cervical mucus changes throughout your cycle. In the first week after your period [when you’re not in your fertile window], there is not much cervical mucus at all.” Clever, eh?
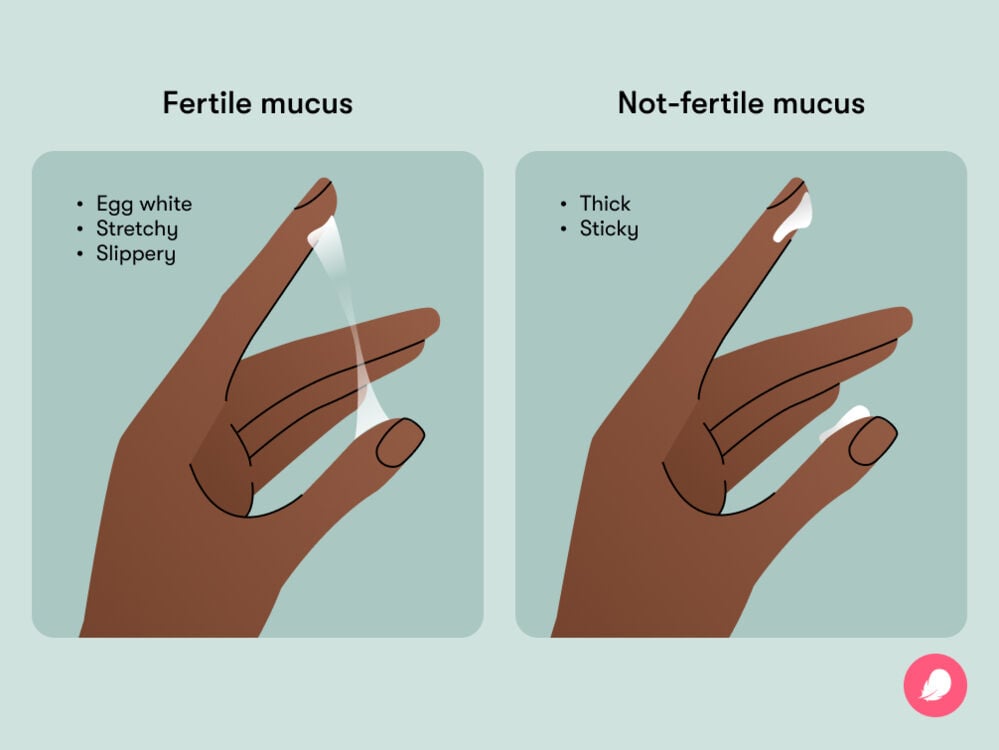
Different types of cervical mucus
During each cycle, the body works around the clock to prepare for a potential pregnancy. This means the brain and different parts of your reproductive system (think the ovaries, cervix, etc.) are constantly talking to each other to make sure everything is working properly.
The menstrual cycle is broken down into three stages: follicular, ovulation, and luteal. Each one impacts your hormone levels differently, which has a direct impact on the color, texture, and amount of discharge and mucus your body produces. Cervical mucus production is mainly controlled by the hormone estrogen, which is also behind some of the other cycle changes you experience.
Immediately after your period, you’ll typically have “dry days,” when very little discharge is produced, and it’s barely visible on your underwear. After this stage, you’ll probably notice more mucus when you wipe.
“Cervical mucus is very important for our health and fertility,” explains Dr. Boyle. “However, unless you’re looking inside your own vagina with a speculum, it can be hard to tell if what you’re noticing with wiping or on your underwear is from the cervix or the vagina.”
If you're wondering whether a specific cervical mucus is normal and what causes it, Dr. Boyle shares more on why it might look and feel different from day to day.
White cervical mucus
“Cervical mucus usually isn’t white, so if you’re seeing a fair amount of white discharge, it is probably vaginal secretions and not cervical mucus,” she explains. White and creamy discharge is generally a healthy color, and you’re most likely to see it at the beginning and end of your cycle. If you notice any itching alongside thick white discharge, this could indicate a yeast infection and is worth getting checked out.
Watery cervical mucus
“Cervical mucus gradually changes throughout your cycle. Right after your period, it is very scant and not noticeable. It then changes as you get close to ovulation and becomes more and more a slippery, stretchy, raw egg white consistency. Sometimes, this might seem watery, or underwear might seem wetter,” says Dr. Boyle. (You can read more on fertile cervical mucus if you keep scrolling.)
“Any watery discharge that lasts more than just a few days doesn’t seem like normal cervical mucus to me. This could be a sign of an infection or other problem and seems like a good reason to get checked,” Dr. Boyle concludes.
Sticky cervical mucus
“Sticky cervical mucus is very typically seen after ovulation. Progesterone is released by the ovaries after ovulation. It causes the cervical mucus to thicken up and become sticky. This is nature’s way of sealing off the uterus and protecting a developing pregnancy,” says Dr. Boyle. “Sometimes, you might notice this mucus as small sticky clumps in your underwear.”
Thick cervical mucus
As we’ve seen above, thick cervical mucus is typical after ovulation thanks to the increase in the hormone progesterone.
Fertile cervical mucus: What does it look like?
As ovulation approaches, so does your fertile window, when the ovaries are most likely to release an egg. This is usually midcycle, although it can change from month to month. Around this time, you’ll no doubt spot another change in your discharge. Usually, we produce more mucus at this point, thanks to high estrogen levels.
“Fertile cervical mucus is often compared to egg whites. It is very slippery and stretchy. It is usually transparent or clear, but it is not abnormal or a sign of anything dangerous if you see a small streak of blood mixed in with it,” explains Dr. Boyle. The mucus is this texture to help the healthy sperm along on their way to the egg.
After ovulation, the amount of discharge decreases, gets sticky again, and loses its stretchiness in the days leading up to your period. Estrogen levels drop off again, and progesterone takes charge to thicken the uterine lining. If a fertilized egg doesn’t implant into the lining, your period will start in a few days.
How to check cervical mucus for fertility
Now that we know that the glands in our cervix produce the most mucus during our fertile window, tracking discharge changes makes sense if you’re trying to get pregnant.
Why? Well, these changes could help you work out when you’re likely to ovulate and, therefore, when the best time to have sex is. In fact, a 2013 University of North Carolina study of 331 women who were trying to conceive found that those who consistently monitored their cervical mucus were significantly more likely to get pregnant than those who didn’t.
For some people, the changes may not be as obvious as described, and this is also perfectly normal. Monitoring your discharge over a few months could help you start to see the changes. “Most people will note the abundant cervical mucus that happens right before ovulation just with wiping,” explains Dr. Boyle. “Some people also check by inserting their finger in the vagina to check for cervical mucus. It may be easier to notice cervical mucus if you check after having a bowel movement, as bearing down can bring cervical mucus closer to the outside of the vagina.”
An ovulation tracking app like Flo can help take the guesswork out of trying to conceive. You can log changes in your discharge and your cycle dates over a series of months. Then, using artificial intelligence, Flo will help you figure out when your fertile window is likely to fall during your cycle.
Remember: Ovulation predictions should never be used for birth control.
Ovulation discharge chart
Of course, it can be hard to picture exactly what you’re looking for. The chart below breaks down what to expect throughout your cycle when checking your discharge, and how to tell if you've got fertile or not fertile cervical mucus.
Take a quiz
Find out what you can do with our Health Assistant
Things that can affect cervical mucus
Certain medications, health conditions, and hygiene products can have an impact on the cervical mucus your body produces. These include the following:
Prescribed estrogen medications that help with fertility or treat conditions, like thin endometrium, can increase the amount of mucus you produce.
Contraceptives that prevent ovulation, for example the hormonal intrauterine device (IUD) and combined oral contraceptive pills, change your cervical mucus, so you won’t notice egg white discharge around the middle of your cycle while using them.
Being overweight might affect your cycle because fat cells increase the amount of estrogen (and therefore mucus) your body produces throughout your cycle.
A sexually transmitted infection (STI) can impact the quality of your cervical mucus and, in some cases, cause a change in the color and smell of your discharge. Read more about STI testing here.
Vaginal conditions like bacterial vaginosis (BV) and yeast infections (also known as thrush) can cause a change in the color, smell, and quality of your mucus. For example, people with BV might notice that their discharge has a fishy smell. Find out more about what your discharge might be trying to tell you here.
Some endocrine disorders, such as polycystic ovary syndrome (a condition that affects the ovaries), can change the levels of estrogen in your body so you produce more cervical mucus on more days of your cycle.
Vaginal douching is “not recommended, as it is harmful to good vaginal health and can disrupt cervical mucus,” according to Dr. Boyle.
When to seek medical help for cervical mucus
If you’re concerned about changes to your cervical mucus or vaginal discharge, speak to your health care provider. Likewise, if you spot any possible signs of infection, it’s a good idea to speak to someone. Such signs can include cervical mucus that’s yellow, green, or gray; causes itchiness or burning; or has an odor. Your health care provider will be able to advise you on any medication-related questions, give you the information you need, and run some tests if necessary.
Cervical mucus: The takeaway
We know now that cervical mucus comes from the glands in and around your cervix and plays a vital role in conception. That’s why it’s important to pay attention to it. Cervical mucus is slightly different for everyone, but keeping track of changes in the color, texture, and amount of mucus in your discharge can help indicate when you’re most fertile or if anything is off with your reproductive health.


Hey, I'm Anique
I started using Flo app to track my period and ovulation because we wanted to have a baby.


The Flo app helped me learn about my body and spot ovulation signs during our conception journey.


I vividly
remember the day
that we switched
Flo into
Pregnancy Mode — it was
such a special
moment.
Real stories, real results
Learn how the Flo app became an amazing cheerleader for us on our conception journey.
References
Bigelow, Jamie L., et al. “Mucus Observations in the Fertile Window: A Better Predictor of Conception than Timing of Intercourse.” Human Reproduction, vol. 19, no. 4, Apr. 2004, pp. 889–92.
Dağ, Zeynep Özcan, and Berna Dilbaz. “Impact of Obesity on Infertility in Women.” Journal of the Turkish German Gynecological Association, vol. 16, no. 2, June 2015, pp. 111–17.
Evans-Hoeker, Emily, et al. “Cervical Mucus Monitoring Prevalence and Associated Fecundability in Women Trying to Conceive.” Fertility and Sterility, vol. 100, no. 4, Oct. 2013, pp. 1033–38.e1.
Katz, D. F. “Human Cervical Mucus: Research Update.” American Journal of Obstetrics and Gynecology, vol. 165, no. 6, Dec. 1991, pp. 1984–86.
“Vaginal Discharge.” Sutter Health, www.sutterhealth.org/health/teens/female/vaginal-discharge. Accessed 13 Jan. 2023.
“Vaginal Discharge Color: What’s Normal and What Isn’t.” Cleveland Clinic, 29 July 2022, health.clevelandclinic.org/vaginal-discharge-mean/.




